INTRODUCTION
University students are highly vulnerable to psychotropic drug use and mental disorders such as anxiety and depression (Amaral et al., 2021; Jenkins et al., 2020; Limone & Toto, 2022). Anxiety is a human characteristic designed to ensure self-preservation. However, in pathological anxiety, symptoms occur more intensely and frequently, causing enormous suffering and harm in everyday life, such as substance abuse and school dropout (Leão et al., 2018). Depression is a chronic, recurrent mood disorder, characterized by sadness, guilt, pessimism, loss of appetite, difficulty concentrating, decreased libido, and increased irritability, negatively affecting the personal lives and academic context of university students (Ribeiro et al., 2014).
University life entails changes in students’ habits, the acquisition of new responsibilities, and exposure to risk factors, including alcohol and tobacco, increasing the likelihood of developing mental disorders in this population (Fauzi et al., 2021; Islam et al., 2022; Ramón-Arbués et al., 2020).
Studies have found a 30.6% prevalence of depression in this population, as opposed to 9% in non-university students (Demenech et al., 2021; Kang et al., 2021; Knapstad et al., 2021; Ibrahim et al., 2013). A systematic review of the global prevalence of anxiety among university students identified a prevalence of 33% in Asia, 51% in Europe and 56% in the United States (Liyanage et al., 2021).
A study conducted in Brazil of 476 freshmen found that 36.1% had anxiety and 28.6% depression (Leão et al., 2018). Other studies have observed a high prevalence of mental disorders during university education, including common mental disorders (CMD) (Gebreegziabher et al., 2019; Karyotaki et al., 2020; Sousa et al., 2021).
CMDs are classified as non-psychotic mental disorders, with symptoms such as insomnia, difficulty concentrating, forgetfulness, fatigue, irritability, feelings of worthlessness and somatic complaints (Gebreegziabher et al., 2019; Risal, 2012; Sousa et al., 2021). When CMD affects young adults such as university students, it can significantly interfere with their relationships, work, and performance of daily activities, compromising their social interactions with family and colleagues (Melese et al., 2016). In the university context, it has a major impact and can lead to students dropping out of courses with long-term social and financial consequences for employment and financial security (Leach & Butterworth, 2012).
These aspects can lead students to use psychotropic drugs to relieve the symptoms resulting from mental suffering. Psychotropic drugs are substances that act on the Central Nervous System (CNS) causing psychological changes that can affect behavior, mood and/or cognition. Due to these effects, psychotropic drugs are among the main means of treating psychiatric disorders (Reis et al., 2021).
The literature shows that university students not only use psychotropic prescription drugs but also self-medicate (Benson et al., 2015; Papazisis et al., 2017). Studies have found that the most used psychotropic drugs by this population are anxiolytics, antidepressants, and amphetamines (Balayssac et al., 2018; Fasanella et al., 2022; Maidana et al., 2020). Although psychotropic drugs are intended for those suffering from mental disorders such as anxiety and depression, some of these drugs can be addictive and should only be used when medically prescribed (Jha et al., 2018; Lerner & Klein, 2019).
These aspects underline the impact of anxiety, depression, and psychotropic drug use on university students.However, most studies address these variables in isolation and there are few studies designed to evaluate the mental health of university students in Brazil. This study therefore aims to identify the factors associated with and their correlation with psychotropic drug use, and anxiety and depressive symptoms in university students.
METHOD
Study design/Location
This is a cross-sectional, analytical study undertaken at a public federal university in Brazil. The university has 19 Academic Units and 51 in-person undergraduate courses, including bachelor’s and master’s degrees.
Participants
The population comprised undergraduate students enrolled in in-person courses. The inclusion criteria were being aged 18 or over, and being enrolled in classroom courses, regardless of the stage they were at in the latter. Students who failed to complete the questionnaire were excluded. We obtained a sample of 902 students who agreed to take part in the survey and completed the questionnaire in full.
Procedure/Measurements
Students were invited to take part in the survey through individual contact, through an invitation letter sent by the university under study, via the institutional e-mail, to all undergraduate students (n = 15.877). This invitation letter explained the title, objectives, and justification of the survey and at the end of the letter, there was a link to the SurveyMonkey® platform to access the data collection instruments. After the letter of invitation had been sent out, students had a total of 60 days to provide their answers. Initially, the emails were sent, and 30 days were allowed for feedback. After this period had elapsed, new emails were sent with an invitation letter and researchers waited another ten days. After this new deadline, emails were sent weekly until 60 days had elapsed. The final deadline for participation in the survey was given in the last two emails. After this period, surveys were no longer allowed to be submitted.
Data collection took place between July and November 2020. An instrument was designed by the authors to collect sociodemographic, economic, medical history and academic life-related variables, considering general aspects to characterize participants. The question “Do you use psychotropic drugs?” was used to collect data on the outcome variable “use of psychotropic drugs,” with dichotomous “yes” and “no” answers. Participants provided the names of the psychiatric drugs they used, which were subsequently classified by consulting the drug database available on the National Health Surveillance Agency website. The psychotropic drug classification was drawn up using a polytomous categorical variable based on the anatomical and therapeutic groups of the Anatomical Therapeutic Chemical (ATC) Classification. The outcome variables “anxiety symptoms” and “depressive symptoms” were collected using the Mini International Neuropsychiatric Interview (MINI), with dichotomous “yes” and “no” answers. This instrument is a diagnostic questionnaire, compatible with DSM-III-R/IV and ICD-10 criteria (Sheehan et al., 1998). Since the questionnaire is organized into independent diagnostic modules and given the objectives of this study, we used Module A “Major Depressive Episode” (MDE), comprising 12 questions. The answers consist of a dichotomous “yes” or “no” variable, while the questions assess current and past major depressive episodes. Module O “Generalized Anxiety Disorder,” comprises ten questions, with answers in a dichotomous “yes” or “no” variable and questions assessing the current generalized anxiety disorder.
It is worth noting that in this study, the MINI instrument was sent to students together with the other data collection instruments and self-administered, although this is not how it is intended to be administered. The choice of procedure was due to the COVID-19 pandemic, which made it impossible for the researcher to collect data in person at the university.
Statistical analysis
Data were collected in Excel and transferred to the SAS/STAT® 9.4, where they were analyzed using descriptive statistics. The anxiety symptoms, depressive symptoms and use of psychiatric medication variables were considered dependent, while those related to sociodemographic and economic factors, medical history, and academic life were considered independent. The use of psychiatric medication was considered an independent variable when associated with outcomes including anxiety and depressive symptoms.
To verify the hypothesis of association between the variables, the data were submitted to Pearson’s Chi-square test and Fisher’s exact test. The hypothesis of association was considered significant when “p” was less than or equal to .05. Logistic regression was used to verify the effect of the independent variables in relation to the dependent ones. The strength of this association was measured using logistic regression models, with odds ratios being calculated with 95% confidence intervals. The logistic regression model used the following dependent variables: current depressive symptoms, anxiety symptoms and psychotropic drug use and independent variables showing a significant association with outcomes, using Pearson’s chi-square test or Fischer’s exact test. The choice of logistic regression is justified in this case is justified because the dependent variables are qualitative and categorical.
Ethical considerations
Data were collected after approval by the Research Ethics Committee of the proposing institution (CAAE 25989119.8.0000.5393), and the co-participating institution (CAAE 25989119.8.3016.5147). Participants signed a Free and Informed Consent Form (FICF), in accordance with Resolution 466/2012 of the National Health Code. The study was conducted in accordance with the World Medical Association International Code of Ethics (Declaration of Helsinki).
RESULTS
In this study, the variables related to sociodemographic profile, economic factors, medical history and academic life were independent, while psychotropic drug use and anxiety and depressive symptoms were dependent variables.
The sample consisted of 902 students. Most of the sample were female (66.4%), with an average age of 24.8 years (SD= 7.7), ranging from 18 to 69 years, white (63%), heterosexual (68.1%), single (88.4%), childless (92.6%), lived with their families (77.8%), did not earn an income (57.7%), full-time students (52.3%) and did not profess any religion (42.3%).
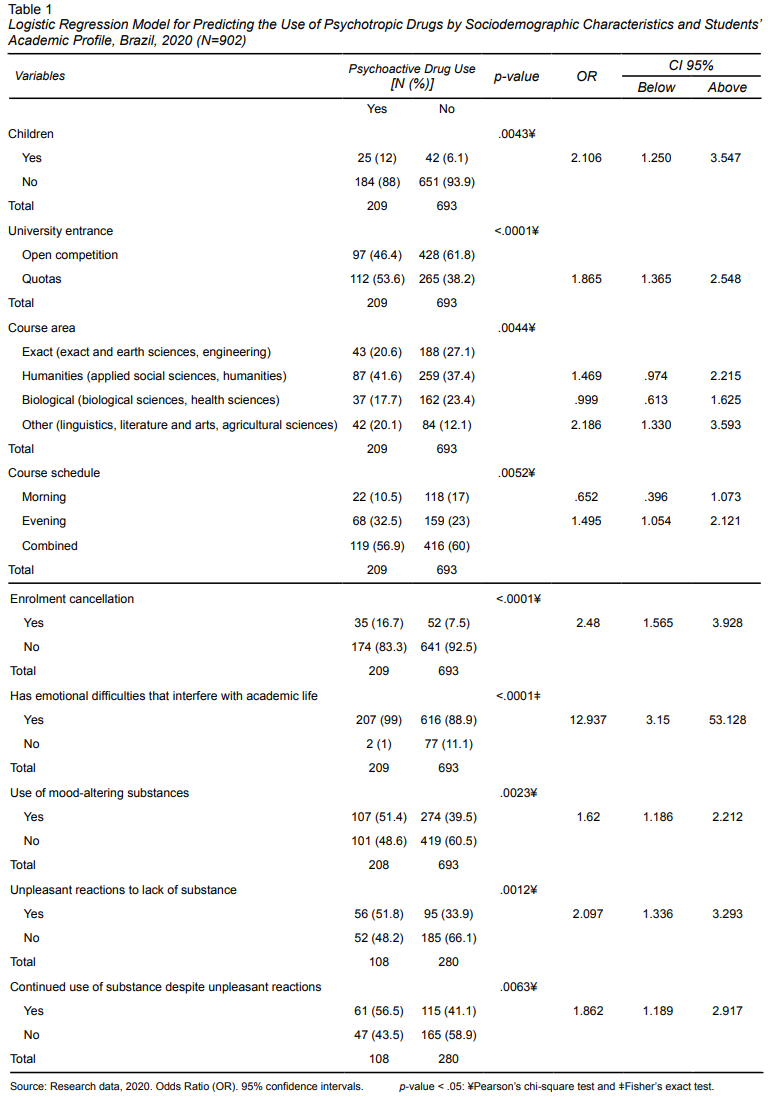
Two hundred and ten (23.3%) students declared that they were currently using psychotropic drugs. Of this group, 105 (50%) reported using at least one psychotropic drug while 70 (33.3%) used two (2). It was striking that 16.7% of participants mentioned using three (3) or more psychotropic drugs. Antidepressants were the most frequently mentioned psychotropic drugs used by the students, n = 193 (21.4%), followed by anticonvulsants/mood stabilizers n = 71 (7.8%). Forty-eight (5.3%) students mentioned using anxiolytics, n = 22 (2.4%) reported using antipsychotics, and 8 (.8%) reported using psychostimulants and nootropics. One hundred and twenty-two (35%) participants had been using psychotropic drugs for less than a year. Most students had been using these drugs for one to two years while 79 (23%) mentioned having used psychotropic drugs for over two years. At the same time, 74% of psychotropic prescriptions were written by psychiatrists, and 6% by neurologists. However, 12% of participants did not inform the doctor prescribing the psychotropic drug that they were using it. One alarming result was that 13.3% of participants stated that they had been using psychiatric medication without a medical prescription. Of this group, 46.4% reported that they had purchased the drugs without a prescription from a pharmacy with 85.7% mentioning anxiety/depression/insomnia as the reason why they used these [SS1] non prescription drugs
In regard to the factors associated with the use of psychotropic drugs, it was found that students who had children were 2,206 times more likely to use psychiatric drugs than students who did not. Students admitted through the quota system were 1,865 times more likely to use psychiatric drugs than those who had entered through the open competition system. University students studying linguistics, literature, arts, and agricultural sciences were 2,186 times more likely to use psychiatric medication than those studying exact, human or biological sciences. Participants who had been forced to cancel their enrolment were 2,480 times more likely to use psychiatric medication. University students who had emotional difficulties that interfered with their academic life were 12,937 times more likely to use psychotropic medication. Students who reported using mood-altering substances (those with the potential to cause dependence) were 1,620 times more likely to use psychiatric drugs. Students who reported unpleasant reactions to the absence of a mood-altering substance were 2,097 times more likely to use psychiatric drugs, while those who continued using a mood-altering substance despite the unpleasant reactions were 1,862 times more likely to use psychiatric drugs than students who stopped using a mood-altering substance due to the unpleasant reactions they experienced. At the same time, students who attended university during the morning shift were .652 times less likely to use psychiatric drugs than those who attended university during the evening shift (Table 1).
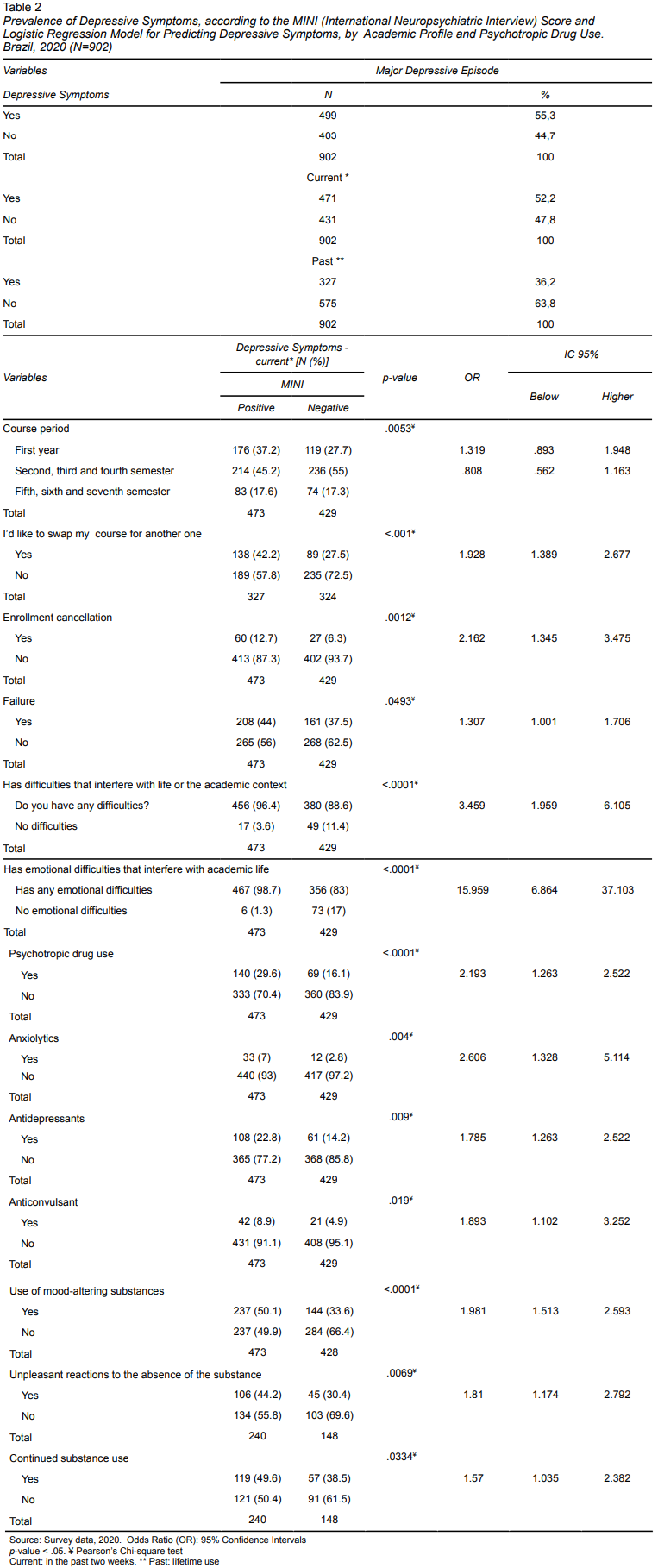
An analysis of participants’ responses to the MINI questionnaire showed that most students had depressive symptoms (n = 499) (55.3%), 52.2% of which reported current depressive symptoms and 36.2% of which reported previous depressive symptoms (Tables 2 and 3).
It was found that students enrolled in the first year of undergraduate courses were 1,319 times more likely to have depressive symptoms than those enrolled in the fifth to seventh semester of their respective undergraduate courses. Conversely, students enrolled in the second to fourth semester were .808 times less likely to have depression symptoms than those enrolled in the fifth to seventh semester of their undergraduate courses. University students who expressed an interest in changing their course were 1.928 times more likely to have depression symptoms while those who were forced to drop out of theirs were .0012 times more likely to have depression symptoms. University students with problems that interfered with their academic life were 3,459 times more likely to have depression symptoms. Students who had emotional difficulties interfering with their academic life were 15,959 times more likely to have depression symptoms. Students who used psychiatric medication were 2,193 times more likely to have depression symptoms, those who used anxiolytics were 2,606 times more likely to have depressive symptoms and those who used antidepressants were 1,785 times more likely to have depressive symptoms than those who did not. In turn, students who used anticonvulsants/mood stabilizers were 1,893 times more likely to have depressive symptoms than those who did not use this type of medication. Students who used mood-altering substances were 1,981 times more likely to have depression symptoms. Those who reported unpleasant reactions when they quit using a mood-altering substance or reduced the amount they took were 1,810 times more likely to have depression symptoms, while those who continued using a mood-altering substance despite the unpleasant reactions it elicited were 1,570 times more likely to have depression symptoms than those who stopped using the mood-altering substance due to the unpleasant reactions it caused (Table 2).
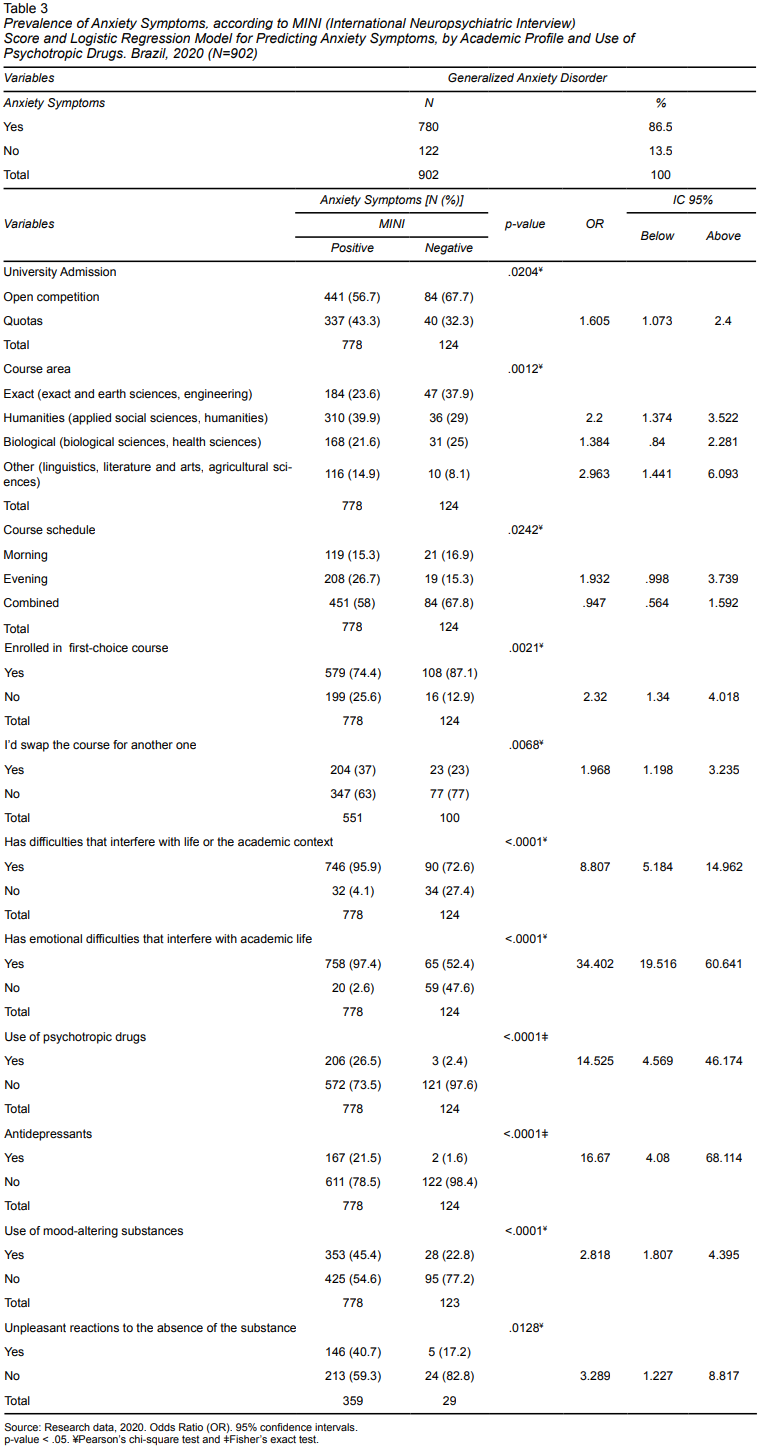
Most students were found to have anxiety symptoms (n = 780) (86.5%). Students admitted to university through the quota system were 1,605 times more likely to have anxiety symptoms than those who entered through the open competition system. University students studying agricultural sciences, literature, art and linguistics were 2,963 times more likely to have anxiety symptoms than those studying exact and biological sciences, while those studying during the evening shift were 1,932 times more likely to have anxiety symptoms. Conversely, studying full-time was identified as a protective factor for anxiety symptoms, with full-time students being .974 times less likely to have anxiety symptoms than those who only studied during the morning or evening shifts. Students enrolled in courses that had not been their first choice were 2,320 times more likely to have anxiety symptoms while those who expressed an interest in changing their university course were 1,968 times more likely to have anxiety symptoms than those who did not. Students with emotional difficulties that interfered with their academic life were 34,402 times more likely to have anxiety symptoms, while those who used psychiatric medication were 14,525 times more likely to have anxiety symptoms. Conversely, students who specifically used antidepressant medication were 16,670 times more likely to display anxiety symptoms than those who did not. Students who reported using mood-altering substances were 2,818 times more likely to have anxiety symptoms while those who reported unpleasant reactions to the lack of these mood-altering substances were 3,289 times more likely to have anxiety symptoms than those who reported no unpleasant reactions to the reduction or lack of mood-altering substances (Table 3).
DISCUSSION AND CONCLUSION
It was striking that nearly a quarter of students used psychotropic drugs. The use of medication in an academic environment, including psychotropic drugs, has become increasingly common, as it is a place with a heavy workload and studies, with the potential for students and teachers to become ill. The rates observed in our study are higher than those identified in the literature, indicating a prevalence of between 10% and 19.7% of psychotropic drug use in this population (Naser et al., 2021).
Most of the participants who used psychotropic drugs had been using them for a year or more. The length of time psychotropic drugs have been used is a significant aspect, especially in the case of benzodiazepines. In this study, 5.3% of psychotropic drug users used benzodiazepines. A study on the risks associated with the abuse of benzodiazepines concluded that continuous, heavy use of these drugs can affect both the health and everyday lives of users. It found that using them for over 26 days exposes users to the risks of withdrawal, tolerance or dependence (Silva et al., 2022), and there is a need for the health team to inform users of the effects of prolonged use, when a prescription is required.
It is worth noting that 13% of students using psychotropic drugs reported using them without a medical prescription, meaning that they self-medicate. Self-medication is understood as the act of ingesting medication on one’s own, without any indication and/or monitoring by a qualified healthcare professional. A meta-analysis review with studies of several countries, including Brazil, showed an overall prevalence of self-medication of 70.1% among university students (Behzadifar et al., 020). In regard to the means of acquiring psychotropic drugs without a medical prescription, even though this medication is intended for controlled use, with prescriptions being retained by pharmacies at the moment of purchase, there was a high frequency of students who purchased them over the counter at pharmacies (46.4%), highlighting the weaknesses in the system for dispensing this type of medication. Most students sought psychotropic drugs without a medical prescription to relieve their anxiety/depression/insomnia symptoms (24) (85.7%). These findings are corroborated by the literature, as research reports that the main reasons leading students to seek psychotropic drugs are recreational use, self-medication (for stress relief and relaxation), pain management, and enhancing academic performance (Naser et al., 2021). At the same time, there is a surprisingly low use of psychostimulants (.8%). This finding can be justified and should be viewed with caution since participants may not have recognized substances such as caffeine, cocaine, and ecstasy as stimulants.
In this study, although 74% of psychotropic prescriptions were written by psychiatrists, 12% of participants failed to inform the professional responsible for the prescription that they would be using them. This finding deserves to be highlighted, because although the benefits of correctly using psychiatric medication are indisputable, treatment and solving the problem should not focus solely on medication. Treatment should be linked to drug therapy and psychotherapy. Furthermore, knowledge about the prescribed medication is essential, as it increases the confidence, safety, and effectiveness of the therapy, as well as reducing side effects and drug interactions (Reis et al., 2021).
Students with children were more likely to take psychotropic drugs. One possible explanation for this finding could be the potential overload resulting from simultaneous activities, such as academic life and child-raising. In this respect, it is worth remembering that most participants in this study were female. A study shows that being a mother and a student requires performing multiple tasks with a direct and indirect influence, both positive and negative, on social, emotional, family, and educational life. Reconciling the roles of mother and student entails difficulties than can lead to absence from classes, withdrawing from courses and even dropping out (Santos, et al., 2021).
Students who entered through the quota system were more likely to use psychotropic drugs as were full-time students. For both quota and full-time students, seeking psychotropic drugs may be associated with financial conditions. The literature shows that low family income can trigger concerns in students, hindering academic performance and creating mental suffering, which can result in the use of psychotropic drugs. It is worth noting that full-time students have greater difficulty securing extra-academic work, limiting their ability to earn an income, resulting in financial difficulty for certain students (Santana et al., 2018).
Dropping out of a course was associated with psychotropic drug use. One study found that psychological distress was the most common reason university students gave for failing to complete a course (Ribeiro et al., 2016). Likewise,, another study found that one of the strategies used by students to cope with suffering and psychological illness was the use of psychotropic drugs (Reis et al., 2021).
There was a greater likelihood of psychotropic drug use among students who reported using mood-altering substances, had unpleasant reactions to quitting and mentioned continuing to use a substance despite the reactions it caused. Starting university can be a period of great vulnerability for the onset and maintenance of use of psychoactive substances (PAS), such as alcohol and tobacco (Barros & Costa, 2019). A study assessing substance use by students found excessive use of alcohol, illicit drugs, stimulants and over-the-counter medication (Boulton & O’Connell, 017). These findings reflect the high levels of use and abuse of licit and illicit psychoactive substances among Brazilian university students, possibly reflecting the teaching model followed and university life (Batista et al., 2022).
Unpleasant reactions to quitting drug use are to be expected following the abuse of dependence-producing substances. Studies show that the use of alcohol, tobacco, drugs and non-prescription medicine among students can damage their health and interfere with their academic performance (Batista et al., 2022; Benson et al., 2015), particularly in situations where students already shows signs and symptoms of withdrawal and dependence.
The prevalence of depression and anxiety symptoms among undergraduate students was 55.3% and 86.5% respectively. In regard to depression symptoms, the result lies within the prevalence range of findings in the literature, which varied from 22.3% to 58.5%. The prevalence of anxiety symptoms was higher than in previous studies, where it varied from 15.8% to 62.9%, depending on the type of instrument used (Naser et al., 2021; Shao et al., 2020). A possible explanation for the high prevalence of anxiety symptoms in participants could be that data were collected during the COVID-19 pandemic. During this period, students were forced to adapt to a new way of learning through virtual platforms, and there was isolation and social distancing, which, according to the literature, contributed to increased screen time, and changes in eating habits and physical activity levels (Barros et al., 2021), as well as anxiety, depression and stress levels (Silva et al., 2021).
In this study, 44% of students failed their exams, and were 1.3 times more likely to have depressive symptoms. Similar results were observed in a study in which just over half the students failed their exams and were 2.6 times more likely to have depressive symptoms than those who regularly passed them (Paudel et al., 2020). The presence of mental disorders among university students interferes with their psychosocial well-being and interpersonal relationships, directly influencing their academic and professional performance (Conceição et al., 2019). In this study, dropping out was associated with the presence of depressive symptoms.
Dissatisfaction with a course was another factor associated with anxiety and depressive symptoms. Research has shown that students’ greatest dissatisfaction with the course they were enrolled in was due to the teaching staff and curriculum structure (Souza & Reinert, 2010). In this respect, one study identified the following as predictors of student satisfaction with the course: teacher training, use of appropriate methodologies, up-to-date teaching methods, coherence, and organization of subject content (Hirsch et al., 2015).
Dissatisfaction can result in emotional imbalance, including nervousness, irritability, impatience, withdrawn behavior, apathy, demotivation, and stress (Hirsch et al., 2015). These aspects should be considered by the management of higher education institutions to prevent mental health problems among undergraduates and improve the teaching-learning process.
This study found that emotional and general difficulties interfered with students’ academic life and context and were related to the presence of depression and anxiety symptoms. A study shows that when students are admitted to higher education institutions, they require emotional and cognitive resources to adapt to the university environment (Padovani et al., 2014). Other studies also note that the stress, mood swings and conflicts experienced during undergraduate studies can interfere with academic performance and even lead to psychological disorders such as anxiety and depression (Santos et al., 2021).
This study found an association between depressive symptoms and the use of psychotropic drugs and mood-altering substances. In this respect, a study has shown that due to attention-related difficulties, dissatisfied academics may experience depressive symptoms and therefore seek an immediate solution through stimulant medication (Benson et al., 2015).The use of psychotropic drugs and substances to feel better or improve one’s mood has also been associated with anxiety symptoms. The literature indicates that tranquilizer and sedative use and abuse is associated with attempts by students to reduce the anxiety caused by academic life and improve sleep quality (Bennett & Holloway, 2017).
An association was found between having unpleasant reactions to the absence of a mood-altering substance and having anxiety symptoms. This aspect can partly be explained by the use of psychoactive substances that cause dependence and tolerance, and anxiety symptoms can occur when use is abruptly interrupted (Prince et al., 2013).
A significant association was also observed between anxiety symptoms and admission through quotas. One possible explanation could be the financial difficulties experienced by these students during their undergraduate studies. A study revealed that students with a significant financial burden had more anxiety symptoms (Shao et al., 2020). Another explanation could be the difficulty of social inclusion experienced by quota students (Santos et al., 2023).
Students enrolled in their second-choice course who were intending to change courses were more likely to display anxiety symptoms. A possible explanation for this finding could be the dissatisfaction of studying a course to pursue an unwanted profession. A study exploring the association between students’ mental health and dissatisfaction with their courses showed that nearly half the students investigated were not studying their degree course of choice. Students’ reports reflected enormous dissatisfaction with their degree courses, the most frequent complaints being anxiety, depression, discouragement about their studies and apathy, risk factors for their health and continuing their studies (Garbin et al., 2020).
The results of this study must be interpreted considering its limitations. A key aspect is that the data were drawn from non-probabilistic sampling. Aspects related to the abuse of psychotropic drugs and the risk of dependence on the latter were not assessed, an issue which future studies could address. Another relevant aspect is that the MINI is designed to be administered by a trained professional, but since data collection was undertaken during the pandemic, it was used as a self-report instrument.
It is essential to recognize that the impact on the mental health of undergraduates can last beyond the pandemic period. Previous studies have shown that crises such as pandemics have lasting effects on the psychological health of the populations affected (Galea et al., 2020; Ornell et al., 2020). Continuing research into the long-term effects on undergraduate mental health, even after the pandemic has ended, is crucial to fully understanding the impact of these events and informing preventive and interventional mental health policies to mitigate future negative impacts.
This study highlights the need for more in-depth assessment of these mental disorders, the use of over-the-counter psychotropic drugs, and other aspects related to academic life, to help students. Higher education institutions currently have departments responsible for the psycho-pedagogical monitoring of students to improve their academic performance, and identify cases in which referrals to specialized professionals are required. However, it is essential to develop interventions such as monitoring and support for students, student counseling, and anxiety management workshops, to detect, manage, monitor, and refer at-risk students at higher education institutions.