INTRODUCTION
Cognition is the mental capacity of an individual to understand and solve everyday problems based on perception, language, reasoning, and sensory abilities (Moraes et al., 2010). Conversely, cognitive decline (CD) is a decline in intellectual abilities, affecting key areas such as memory, language, learning, and the performance of everyday tasks and behavior (De Ronchi et al., 2005; Machado et al., 2011). This condition has an impact in terms of reduced functional capacity, independence, and autonomy, affecting the quality of life and causing psychosocial damage (Machado et al., 2011; Pavel et al., 2023).
CD derives from the normal process of aging or the transition to dementia, a chronic condition characterized by the presence of CD affecting a significant portion of the older population (Machado et al., 2011; Trindade et al., 2013). As a result of the aging process, the number of individuals exposed to CD gradually increases, significantly impacting public health (Lira & Santos, 2012; Rosa et al., 2018). The global prevalence of CD in community-dwelling older adults ranges from 5.1% to 41% (Pais et al., 2020). In Brazil, however, this prevalence exceeds 50% in older adults treated in Primary Health Care (PHC) (Pereira et al., 2020).
CD can manifest itself during aging and is proportional to advancing age, causing a decline in the structures responsible for the normal functioning of brain systems (De Ronchi et al., 2005). In addition to age, other determinants of CD include educational attainment, sex, social support, lifestyle, and marital status (Wu et al., 2011; Pereira et al., 2020; Horacio et al., 2021). Moreover, this situation can be exacerbated by food insecurity (FI), a condition that can be acute or chronic, and results from a lack of regular, sufficient access to food in terms of quantity and quality.
FI is a shortage of the food and nutrients (protein with high biological value, vitamins, minerals, and fiber) essential to maintaining health, which can lead to poor nutritional status and mental health (Martin et al., 2007; Frongillo et al., 2017; Koyanagi et al., 2019). In addition, FI may lead to stress, which can trigger the onset of CD (Smith et al., 2021). Food insecurity (FI) is believed to cause multisystemic physiological dysregulation (an increase in allostatic load), caused by nutrient deficit and chronic stress. The immune and metabolic systems are most severely affected, causing inflammatory and neuroendocrine damage that disrupts homeostasis and may impair cognition (Pak & Kim, 2021; Wilbrecht et al., 2024). Conversely, an adequate diet is a protective factor for the preservation of cognitive functions, enhancing the ability to perform daily activities (Martin et al., 2007).
Despite scientific evidence demonstrating the relationship between FI and CD, there is a dearth of studies analyzing this phenomenon across the levels of FI (mild, moderate, and severe). Moreover, as most research is conducted in high-income (developed) countries, it is essential to understand this situation in settings such as northeastern Brazil, where older adults have higher rates of FI due to vulnerabilities associated with low income and poor education, exacerbated by the shortage of social and health public policies (Geib et al., 2012; Royer et al., 2021).
Given the rapid aging of the population and the lack of evidence on this issue in Latin America, it is necessary to determine the impact of FI, associated with inadequate, irregular dietary habits, on CD. This study therefore sought to understand the association between FI and CD in older adults treated in Primary Health Care in a municipality in the Northeast Region of Brazil.
METHOD
Study Type, Location and Population
This is a cross-sectional study conducted among older adults (aged 60 years and older) living in private households and registered with the Family Health Strategy (FHS), a program linked to PHC in Brazil. The study is part of a larger research project entitled “Health Assessment of Older Adults Living in the Municipality of Barreiras/BA.” The study location was the municipality of Barreiras, located in the Oeste region of the state of Bahia, in the Northeast of Brazil. This article was written in accordance with the guidelines of the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) checklist (Vandenbroucke et al., 2007).
Sample
The study population comprised older adults cared for by 23 FHS teams in the municipality. To calculate the sample size of the matrix project, an overall prevalence of 50%, a margin of error of 5% and a confidence level of 95% were obtained, yielding a total sample of 356 participants. The power of the study was calculated using OpenEpi software (OpenEpi, Atlanta, Georgia). Considering a test power of 67% and a significance level of 5%, the sample of older adults made it possible to identify an odds ratio (OR) of 1.2, with a prevalence of 64% among those exposed and 52% among those not exposed.
Sampling was carried out in two stages: 1) random and stratified with proportional allocation and 2) simple random. In the first stage, a calculation was made according to the number of older adults in the strata (23 territories covered by the FHS teams), which, in addition to proportionality, ensured the representativeness of the territories; 2) in the second, the sampling was simple random. Based on the number in each stratum, the older adults in each FHS team were chosen by lot and a nominal list of the interview candidates obtained.
Inclusion and exclusion criteria
Eligible participants were older adults aged 60 years and over, of either sex, living in the urban area, registered with the FHS and chosen by lot, who agreed to participate by signing an informed consent form (ICF). Older adults with health conditions that prevented them from traveling to the data collection site were excluded, as were those with severe cognitive impairment, as identified by the FHS teams. In addition, older adults living in long-term care institutions for the elderly or who were hospitalized during the data collection period did not participate.
Data collection
Data were collected from February 2017 to August 2018 at the Family Health Units (FHUs) where the older adults were registered. To make the data collection feasible, prior meetings were held with professionals from each health unit, where details of the survey were presented, such as the equipment, forms, and spaces required. In addition, a list of the older adults selected for the study was given to the Community Health Agents (CHAs). The CHAs were responsible for distributing invitations with basic information on the study, the date and time of attendance, and technical guidelines for conducting the data collection to the older adults
Data collection was undertaken directly with the selected older adults by a standardized, trained team of researchers, comprising university health students. To this end, a previously tested, coded questionnaire was used to obtain general information on the older adults, making it possible to characterize the population in terms of social, economic, demographic, lifestyle, nutritional, and health status variables. In addition, specific scales were used to assess FI and CD.
Outcome
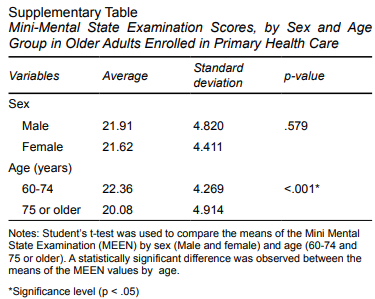
CD was assessed using the Mini Mental State Examination (MMSE), one of the most widely used tools for assessing cognitive function (Folstein et al., 1975). The MMSE assesses dimensions such as language, memory, attention, orientation, and concentration (Bertolucci et al., 1994). In this study, the cut-off points used to classify the absence or presence of CD were defined on the basis of educational attainment. Thus, older adults with MMSE scores < 25 points for literate and < 20 points for non-literate older adults were considered as having CD, since educational attainment is a key determinant influencing cognitive ability. Older adults with MMSE scores ≥ 25 for literate and ≥ 20 points for non-literate older adults were classified as not having CD (Brucki et al., 2003).
Although the MMSE is one of the most widely used instruments for researching CD, it has limitations, particularly because of the social context of older adults. It can also be affected by factors such as educational attainment, income, sex, and age. The evaluative parameters therefore require adjustment for these scenarios, as was done in the study. The lack of a standardized cutoff point is also a significant obstacle, potentially yielding divergent results in similar populations and complicating comparability between studies (Ismail et al., 2010).
Exposure
FI was assessed using the Brazilian Food Insecurity Scale (EBIA), a psychometric scale with 14 dichotomous questions translated, adapted and validated for use in the Brazilian population (Segall-Corrêa et al., 2014; Segall-Corrêa & Marin-Leon, 2015). After the scale had been administered, households with older adults were classified into the following four levels: food security (FS), mild FI, moderate FI, and severe FI, with reference values considering the presence or absence of children under 18 years of age. In other words, in situations without an individual < 18,
a household with an older adult was classified as FS (0 points), mild FI (1-4 points), moderate FI (5-6 points) or severe FI (7-8 points); whereas in those with individuals
< 18 years, they were classified as FS (0 points), mild FI
(1-5 points), moderate FI (6-9 points) or severe FI (10-14 points) (Sardinh et al., 2014).
Covariates
For this study, the demographic and social covariates were as follows: age (60 to 69 years, 70 to 79 years, or 80 years or older), sex (male or female), schooling (< 4 years or ≥ 4 years of study), marital status (partnered or unpartnered), living alone (yes or no), and race/color (white, Asian, Black or people of color). Lifestyle covariates included alcohol consumption (yes or no), smoking (yes or no), and physical activity (yes or no). Participants in physical activity were considered elderly individuals who self-reported (yes) engaging in any level or type of activity. Health and nutritional status covariates included body mass index (BMI) (underweight, normal, or overweight), according to the Pan American Health Organization classification (OPAS, 2002); hospitalization in the past year (yes or no); systemic arterial hypertension (SAH) (yes or no); diabetes mellitus (DM) (yes or no); and dyslipidemia (yes or no). These chronic diseases were self-reported based on medical diagnoses.
Data analysis
SPSS was used to tabulate and analyze the data. To characterize the population studied, the variables were presented using descriptive analyses with frequency distribution (absolute and relative). Data normality was checked using the Kolmogorov-Smirnov test for all the variables analyzed. Pearson’s chi-squared test was also used to check for associations between categorical variables. At this point, the outcome was categorized as with or without CD. Exposure (FI) was categorized as FS or FI. Variables showing statistical significance of less than .20 in the bivariate analysis were included in the multivariate model, together with other adjustment variables (sex and age).
Binomial logistic regression was used to assess the association between CD (with and without) and FI levels (FS, mild FI, and moderate/severe FI). Crude and adjusted odds ratios (ORs) with their respective 95% confidence intervals (95% CIs) were obtained as measures of association. In all the analyses, α = .05 was used to determine statistical significance.
Ethical considerations
The study was approved by the Research Ethics Committee (Verdict No. 1.447.361/2016), in accordance with the rules established by Resolution No. 466/12 of the National Health Council of the Brazilian Ministry of Health. Participation in the study was voluntary and confirmed by participants’ signature or fingerprint on the ICF.
RESULTS
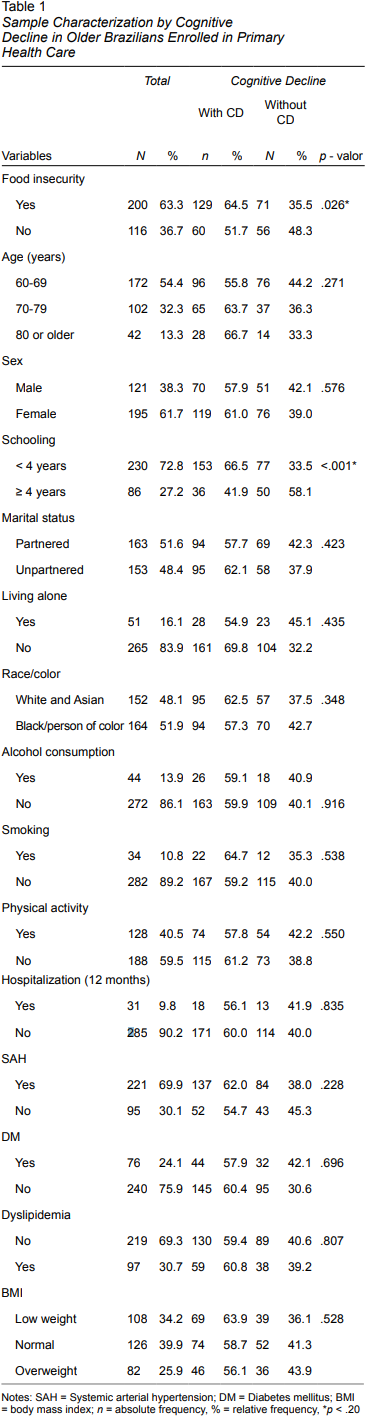
Of the 316 individuals assessed (11.2% losses), 61.7% were female, 54.4% were aged 60 to 69, and 51.9% were Black or people of color. It was also found that 72.8% of the older adults had had fewer than four years of schooling, 51.6% were partnered and 16.1% lived alone. Regarding their health status, 69.9% had been diagnosed with SAH and 34.2% were classified as underweight according to BMI. The prevalence of FI was 63.3% among older adults, with 25.6% experiencing moderate or severe FI. The prevalence of CD was 59.8% (Table 1).
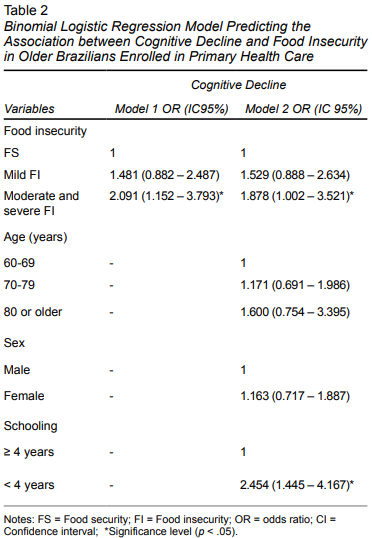
In the bivariate analysis, a statistically significant association was found between FI and CD (p = .026). In addition to FI, CD was also associated with schooling (p = .001) (Table 1). In the logistic regression analysis, after adjustments, a statistically significant association was only observed between households with older adults with moderate/severe FI and CD (OR 1.878; 95%CI 1.002 - 3.521). There was no association between mild FI and CD (OR 1.529; 95% CI 0.888 - 2.634). In the final model, in addition to FI, there was also a statistically significant association between CD and < 4 years of schooling (OR 2.454; 95% CI 1.445 - 4.167) (Table 2). The final model fit was observed through the value obtained in the Hosmer-Lemeshow test (p = .911) and Nagelkerke R square = .088.
DISCUSSION AND CONCLUSION
This study found a statistically significant association between moderate/severe FI and CD in community-dwelling older adults treated in PHC in a municipality in the Northeast of Brazil. It was observed that households with older adults experiencing moderate/severe FI were almost twice as likely to have CD. In other words, more severe FI conditions, characterized by severe limitations on both the quantity and quality of the diet, may be associated with cognitive impairment in community-dwelling older adults.
A systematic review study by Royer et al. (2021)found that FI status is associated with a decline in cognitive function across the lifespan. A similar result was found in a study of older American adults showing an inverse association between FI and cognitive ability (Frith et al., 2018). It is therefore possible to observe a strong relationship between FI and CD in older adults, as cognitive functions such as memory, language, attention, and mathematical problem-solving have been shown to be more impaired in older adults with FI. At the same time, older adults with FS may have a lower risk of CD. A longitudinal study conducted in India with a representative sample assessing various cognitive aspects found that older people with FS were less likely to have word recall problems or computational problems compared to those with FI (Kumar et al., 2021).
This study found that only more severe cases of FI (moderate/severe) were associated with CD. Similar results were observed in a study conducted by Koyanagi et al. (2019) of adult and older adult South Africans, showing that FI, especially in its more severe forms (moderate and severe), is associated with cognitive impairment. Older people with moderate and severe FI were about four times more likely to have CD. A study of adult and older adult Puerto Ricans found an association between more severe levels of FI and lower cognition and a greater likelihood of CD, particularly among the older population (Gao et al., 2009).
FI can contribute to the development of CD through a number of mechanisms, including inadequate food intake and poor diet quality. This is because, in the context of FI, the diet comprises fewer foods with higher nutritional value and greater consumption of ultra-processed foods, leading to nutrient deficiencies (Frongillo et al., 2017; Hutchinson & Tarasuk, 2021). There is a decrease in the consumption of vegetables, fruits, and dairy products, as well as foods that are sources of vitamins A and B-6, calcium, magnesium and zinc (Hanson & Connor, 2014). A study of older adults in Singapore showed that compromised nutritional status, such as malnutrition, is associated with CD, probably due to the lack of nutrients required for brain function and cognition (Chye et al., 2018).
The literature contains evidence of this association between micronutrient deficiencies and CD (Mustafa et al., 2022). Another study of community-dwelling older Brazilian adults found a strong association between CD and zinc deficiency (Marchetti et al., 2022). An integrative literature review indicated that vitamin B12 and folic acid deficiencies are associated with the risk of CD in older adults, due to increases in the concentration of homocysteine and methylmalonic acid, which cause changes in the central nervous system and affect cognition (Sousa et al., 2020). Conversely, an adequate diet, which is usually the case for older adults in a FS situation, consisting of foods such as fruits and vegetables, which are sources of antioxidant micronutrients and anti-inflammatory agents, has been shown to preserve cognition and therefore delay the onset of CD (Gardener & Rainey-Smith, 2018).
Older adults with FI, especially at moderate and severe levels, experience a decrease in the number of meals, the amount of food per meal and therefore a lower intake of macro- and micronutrients (Pereira et al., 2022). In the study conducted by Cardozo et al., (2020), families with moderate and severe FI were 55% and 57% respectively more likely to adhere to a restricted diet, characterized by a lower frequency of consumption of most food groups, including fruits and vegetables. Moreover, families with FI were 41% less likely to adopt healthy eating habits. If a healthy diet is unattainable for those with FI, nutrient deficiencies that fail to protect cognitive function become more likely. This dietary scenario contributes to the development of CD in older adults.
In addition, the experience of FI can lead to mental health damage due to the stress caused by not knowing where their next meal is coming from, mainly due to low socioeconomic status (Pereira et al., 2023). Studies have shown that the experience of FI can cause psychological distress and stress, which, in turn, can lead to changes in brain structures and functions, resulting in the onset or worsening of cognitive impairment (Vilela et al., 2014; Smith et al., 2021). As observed in a longitudinal analysis of adult and older adult Puerto Ricans, FI was significantly associated with higher cortisol levels, hypothalamic-pituitary-adrenal (HPA) axis dysregulation, and sympathetic nervous system markers (Gao et al., 2009).
Repeated stressful situations due to FI increase allostatic load, which causes wear and tear to the body, leading to brain changes that culminate in CD (McClain et al., 2018). The increase in cortisol levels due to stress may increase the desire for more palatable foods, such as foods with a high sugar and fat content, to reduce stress levels, acting as a reward system (Adam & Epel, 2007). There may therefore be a greater tendency to make less healthy food choices as a result of the stress caused by FI. Dietary insufficiency associated with higher levels of FI and the negative effects of this stressful experience may exacerbate CD and the health of older adults with this status.
Despite the methodological rigor of this cross-sectional study, and the results showing an association between CD and FI, it is not possible to make statements about the causality between exposure and outcome. Longitudinal studies on this issue, which are as yet limited, would therefore be required to show the direction of causality between FI and CD. Another aspect to consider was the use of the MMSE, which, although it is the most widely used tool for measuring CD, lacks a standardized cut-off point. Nevertheless, reference values were chosen that were appropriate for the characteristics of the population. Furthermore, it was necessary to exclude older adults with a high degree of CD, since it was impossible to administer the MMSE correctly. Another limitation was the sample size, which probably influenced the power value of the study, calculated post hoc (67%). Although losses in the sample certainly contributed to this condition, they did not affect the representativeness of the sample, since the distribution of losses was not concentrated in specific strata.Moreover, nutritional covariates were not used in this study. This aspect can be considered a limitation in the adjustment of statistical models.
In terms of contributions, it should be noted that this is the first study to address this issue in older Brazilian adults. Another key aspect is the fact that the study focused on community-dwelling older adults treated in PHC. It is also worth noting that FI was analyzed in terms of its different levels, mild and moderate/severe, with the understanding that eating patterns and strategies differ in the various categories of this status.
This study showed that the experience of moderate/severe FI in households with older adults registered with PHC in Brazil may be associated with the presence of CD. In other words, unhealthy dietary patterns, with restricted quantity and quality of food and nutrients, can result in cognitive impairment in older adults. Nutritional deficiencies and mental health effects caused by stress and psychological distress may explain this association. In this respect, given the characteristics of aging and their impact on the health of individuals, FI must be addressed with public policies that facilitate access to sufficient healthy food.