INTRODUCTION
Globally, suicide claims the lives of 45,800 adolescents annually, making it the fifth leading cause of death among individuals aged 10 to 19, the fourth among males aged 15 to 19, and the third among females in the same age group (Fondo de las Naciones Unidas para la Infancia [UNICEF], 2022). In Mexican adolescents aged 15 to 19, the suicide rate totaled 7.7 per 100,000 in 2022, compared to 3.6 in 2017, representing a 114% increase over six years (Instituto Nacional de Estadística y Geografía [INEGI], 2018; 2023).According to UNICEF (2020), eight out of ten youth suicides occur in school settings, making them ideal for the implementation of universal suicidal prevention interventions (Pan American Health Organization, 2023).
Dialectical Behavioral Therapy (DBT), developed by Linehan (1993), is the first treatment for which there is strong evidence that it effectively addresses issues related to dysregulated behaviors, cognition, and emotions (American Psychological Association, 2022), including suicidal behavior. Meta-analyses of the effectiveness of DBT demonstrate that it helps individuals reduce suicidal and self-injurious behaviors, decreases the need for specialized psychiatric services, and reduces treatment dropout rates (DeCou et al., 2019; Panos et al., 2014). Asarnow et al. (2021) found that DBT improved emotional regulation and the use of practical coping skills in adolescents who had attempted suicide.Hermosillo-de-la-Torre et al. (2023) recently obtained comparable results by using a DBT skills program as independent treatment for Mexican adolescents in the initial stages of suicidal thoughts. According to Neacsiu et al. (2014), DBT skills training seeks to equip individuals with empirically grounded strategies to accurately identify and label emotions, decrease emotional vulnerability, modulate emotional intensity, and navigate high-stress situations without resorting to self-destructive behaviors.
Based on previous findings, this study aims to evaluate whether the DBT skills program adapted for Mexican adolescents in school settings reduces the level of suicide risk. Additionally, it seeks to determine whether the use of DBT skills enhances emotional regulation and contributes to the reduction of suicide risk in a sample of Mexican adolescents from three Mexican states.
METHOD
Researchers implemented a multicenter, quasi-experimental, quantitative, pre-post design (Shadish et al., 2002) across four cities in three states in Mexico: La Paz, Baja California Sur; Ciudad del Carmen, Campeche; San Francisco de Campeche, Campeche; and Cuernavaca, Morelos.
Participants
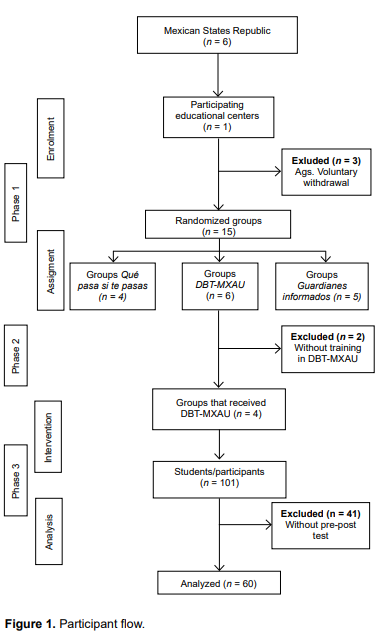
The current study is part of a larger national project approved by the Ministry of Science, Humanities, Technology, and Innovation (SECITHI). It aims to evaluate the effectiveness of three psychoeducational interventions designed to reduce suicide risk among Mexican adolescents attending public middle schools in marginalized urban areas. The researchers conducted the study in three distinct phases. In Phase 1, we screened for risk factors associated with suicide and substance use in middle schools across six states selected for convenience (Figure 1). In Phase 2, we trained state mental health personnel in the intervention programs. In Phase 3, we implemented the intervention programs. This study focuses on the DBTMXAU intervention with four groups assigned to this study located in four cities across three states.
Sixty adolescents aged between 13 and 17 (M = 15.23, SD = 1.59) participated (45% of whom were female, and 53% male, while 2% preferred not to disclose their gender). Participants were enrolled in the third year of middle school. The inclusion criteria were a) being a regular student at the participating school, b) having granted consent to participate in the study, and c) having parental consent.The exclusion criteria were as follows: a) refusal to provide informed consent for participation in the study; b) incomplete or inadequate completion of pre- and post-intervention assessments; c) attendance at fewer than 80% of intervention sessions; and d) presence of hearing or visual impairments.
Measurements
Trait Meta-Mood Scale 24 items (TMMS-24). Adapted for Mexican adolescents by Ocaña et al. (2019), this scale evaluates the perception of socio-emotional skills through three dimensions: a) emotional attention (the degree to which people pay attention to their emotions and feelings); b) emotional clarity (the ability to understand one’s emotional states); and c) emotional repair (the capacity to regulate and manage emotional states appropriately). It is a 5-point Likert scale, where 1 indicates “strongly disagree” and 5 indicates “strongly agree.” The overall scale had internal consistency, with a Cronbach’s Alpha coefficient of α = .910. In the current study, we obtained an α of .87 for the pre-test and .85 for the post-test. The dimensions also exhibited good psychometric properties, with alphas of .85 in emotional attention, .87 in emotional clarity, and .87 in emotional repair.
Dialectical Behavioral Skills Scale (EHSE-DBT). Developed by Acevedo (2021) to assess the use of DBT socio-emotional skills in Mexican adolescents, this scale contains 37 items (six for mindfulness, six for distress tolerance, 15 for emotional regulation, and 10 for interpersonal effectiveness). It includes an Osgood rating scale, in which each item contains bipolar adjective pairs on a scale of 1 to 4, with 1 representing one extreme of a concept and 4 the other. The scale demonstrated acceptable reliability in both pre-assessment and post-assessment, with α values of .80 and .81, respectively.
The Columbia Suicidality Severity Rating Scale (C-SSRS). Developed by Posner in 2008 (no existe link al PDF), identifies individuals at risk of suicide. We used the Spanish version in a self-report format for Chilean adolescents, following the method used by Núñez et al. (2019). The scale comprises seven questions with dichotomous answers: yes or no. We assessed individuals as having low suicide risk if they answered questions 1 and 2 affirmatively. An affirmative answer to question 6 indicated moderate risk, while affirmative answers to questions 4, 5, and 7 were classified as high risk. The analysis showed that the scale had high reliability, with a KR-20 score of .88 for the pre-evaluation and .91 for the post-evaluation after we eliminated question 3.
Procedure
We implemented the DBT-MXAU program with teams of designated mental health professionals from May to July 2023. A total of sixteen psychologists from the mental health sector (12 women and four men) administered the DBT-MXAU program between September and December 2023 in four regions: Morelos (n = 5), Baja California Sur (n = 2), Ciudad del Carmen (n = 6), and San Francisco de Campeche (n = 3). The research team delivered the Educational Transfer Program through an online course hosted on the Moodle platform at https://prevenirelsuicidioadolescente.org. A psychologist recognized by Behavioral Tech taught the course. The training, comprising six asynchronous modules with reading, videos, and practical exercises, focused on the theoretical, epistemological, and operational foundations of DBT. We also conducted eight weekly synchronous sessions during the training. We provided continuous support to facilitators through a WhatsApp group and video calls for answering questions in real time.
The intervention program consists of 11 sessions, the first two being designed to inform and engage participants.It includes two sessions in each skill module, (mindfulness, distress tolerance, emotional regulation, and interpersonal effectiveness). Each session, lasting two hours, features a facilitator and a co-facilitator and follows a structured format that incorporates mindfulness activities, skill reviews, teaching, and homework assignments. The intervention includes a welcome session, four thematic modules, and a closing session, adopting the theoretical and methodological approach of DBT. We developed two key resources as supporting materials, (1) The Guidelines and Framework for DBT-MXAU Trainers, a 190-page guide including theoretical foundations, the program structure, and recommendations for its implementation in school settings, and (2) The DBT-MXAU Skills Training Manual, adapted by Hermosillo-de-la-Torre et al, (2025), which introduces the skills through simple explanations, examples, generalization activities, and visual resources designed for adolescents. This booklet presents DBT-A (Rathus & Miller, 2014) and DBT Skills (Linehan, 2014) specifically for Mexican adolescents experiencing high social vulnerability in urban school settings. During the implementation of the DBT-MXAU program, facilitators actively conducted pre- and post-treatment assessments in both online and paper-and-pencil formats. These assessments measured emotional intelligence, the use of DBT skills, and suicide risk. In addition, we requested video recordings of the sessions for supervision by the research team. After implementing the DBT-MXAU, we organized a meeting with the facilitators to obtain feedback on their experience with the implementation.
Statistical analysis
We conducted all statistical analyses using IBM SPSS Statistics (Version 20), setting a two-tailed alpha level of .05 for significance tests.
Descriptive statistics and prevalence estimates were calculated for sociodemographic, academic, and emotional variables, including means, standard deviations, and 95% confidence intervals. Prevalence rates of suicide risk (global, checklist, and crisis indices) were calculated and stratified by school, sex, and risk level (low, moderate, and high).
Due to the small sample size and non-normal distributions, we used Wilcoxon signed-rank tests to compare pre-and post-intervention scores on (a) the three suicide-risk indices and (b) the emotional intelligence subscales (attention, clarity, and repair), as well as the self-reported frequency of DBT skills. We calculated effect sizes using the formula r = |Z| / √ N , interpreting them as small (.10), medium (.30), or large (.50).
The change in scores (Δ = post − pre) was calculated for each outcome and examined with the Kruskal–Wallis test across the four schools (three states). Effect magnitude was indexed by η2;_H = H / (N − 1) and classified as trivial (.01), small (.06), or medium (.14), according to Tomczak & Tomczak (2014).
The study assessed the relationships between the use of DBT skills, emotion regulation, and suicide risk following the intervention using Spearman’s rho (ρ), interpreting effect sizes as small (.10), medium (.30), or large (.50).
We conducted ordinal logistic regressions using the PLUM procedure with a cumulative logit link. In Model A, we assessed whether the city of residence influenced the post-intervention suicide risk category. In Model B, we examined how the frequency of DBT skills and emotional repair after the intervention predicted risk categories, controlling for baseline risk. Each model included a test of parallel lines to verify the proportional odds assumption.
Ethical considerations
The Bioethics Committee of the National Institute of Public Health approved the study, with folio number CI:1742, Folio 107. We informed each participating adolescent and their parents about the goals and scope of the program. After they had understood the objectives, the adolescents voluntarily decided whether they wished to participate. Those who chose not to participate in the program, or decided to discontinue their attendance, were given alternative activities determined by school authorities. Additionally, we referred adolescents identified as being at high risk for suicide to appropriate psychological care services through the Ministry of Health.
RESULTS
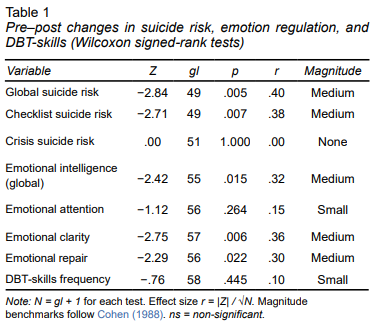
A series of Wilcoxon signed-rank tests revealed that the DBT-MXAU produced meaningful reductions in suicide-risk indices. Students’ overall risk scores declined significantly from pre-intervention to post-intervention, Z = −2.84, p = .005, r = .40, indicating a medium effect. A parallel analysis using the program-checklist (PC) risk indicator yielded a similar result, Z = −2.71, p = .007, r = .38. Conversely, crisis-specific suicide-risk scores remained unchanged, Z = .00, p = 1.00, r = .00. Together, these findings suggest that the intervention was effective in lowering general and checklist-based suicide risk yet failed to modify crisis-level risk in this sample of Mexican adolescents. DBT skills frequency remained stable whereas global emotional intelligence rose significantly. According to Cohen’s benchmarks, the significant effects were small to medium in magnitude (Table 1).
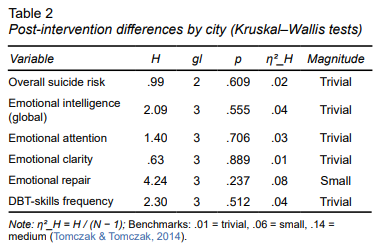
The Kruskal–Wallis tests showed that post-intervention outcomes varied as a function of participants’ city of residence (four groups). None of the contrasts achieved statistical significance: overall suicide-risk scores, χ2; (2) = .99, p = .61; global emotional-intelligence scores, χ2; (3) = 2.09, p = .56; emotional attention, χ2; (3) = 1.40, p = .71; emotional clarity, χ2; (3) = .63, p = .89; emotional repair, χ2; (3) = 4.24, p = .24; checklist-based attention, χ2; (3) = .78, p = .85; checklist-based clarity, χ2; (3) = 2.13, p = .55; checklist-based repair, χ2; (3) = 2.17, p = .54; and overall DBT-skills frequency, χ2; (3) = 2.30, p = .51. (Table 2).
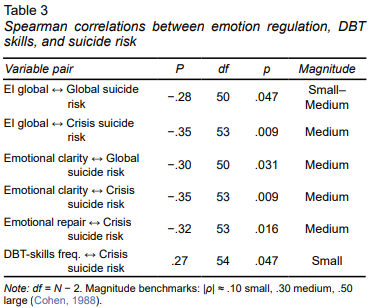
Spearman’s rank-order correlations showed positive interrelations among the emotion-regulation facets: global emotional intelligence correlated with emotional attention (ρ = .87, p < .001), clarity (ρ = .84, p < .001), and repair (ρ = .84, p < .001), and the subscales themselves were moderately intercorrelated (ρs = .57–.62, all ps < .001). Higher scores on several emotion-regulation indices were associated with lower suicide risk levels. Emotional clarity correlated negatively with both overall suicide risk (ρ = –.30, p = .031, n = 52) and crisis-level risk (ρ = –.35, p = .009, n = 55), while emotional repair showed a similar inverse association with crisis-level risk (ρ = –.32, p = .016, n = 55). Global emotional intelligence displayed small but significant negative links to overall risk (ρ = –.28, p = .047) and crisis-level risk (ρ = –.35, p = .009). In contrast, emotional attention was unrelated to either suicide risk (|ρ| ≤ .21, ps > .11). Post-intervention DBT-skills frequency did not correlate with global emotion-regulation scores (|ρ| ≤ .06, ps > .70) or overall suicide risk (ρ = –.01, p = .964). (Table 3).
An ordinal logistic regression was conducted to determine whether the city of residence influenced adolescents’ suicide risk levels following the intervention. The analysis included a total of 52 valid cases. Model fit statistics indicated that adding the predictor failed to enhance the intercept-only model, as shown by Δχ2; (1) = .03, p = .873, resulting in a negligible amount of explained variance (Nagelkerke R2; = .001). Overall, the model fit was deemed acceptable, (χ2; = 2.00, df = 3, p = .572, and Deviance χ2; = 2.93, df = 3, p = .403).
The location parameter for the city of residence was not significant, with a coefficient of b = -.08, standard error (SE) = .52, Wald χ2; (1) = .03, p = .874, and a 95% confidence interval of [−1.11, .94], corresponding to an odds ratio of .92.
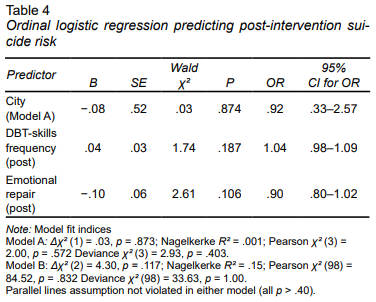
An ordinal logistic regression suggested that post-intervention DBT-skills frequency (HDBT_POST) and emotional repair (REP_E_POST) predicted adolescents’ suicide-risk category (RS_POST_1; 0 = no risk, 1 = low risk, 2 = moderate risk). The outcome was markedly skewed (90.4 % in the no-risk category), resulting in 66.7 % empty predictor–outcome cells. Nevertheless, overall model fit was adequate (Pearson χ2; = 84.52, df = 98, p = .832; Deviance χ2; = 33.63, df = 98, p = 1.000). Adding the two predictors did not improve the intercept-only model, Δχ2; (2) = 4.30, p = .117, and explained little variance (Nagelkerke R2; = .15).Neither DBT-skills use, b = .04, SE = .03, Wald χ2; (1) = 1.74, p = .187, 95 % CI [−.02, .09], OR = 1.04, nor emotional repair, b = −.10, SE = .06, Wald χ2; (1) = 2.61, p = .106, 95 % CI [−.23, .02], OR = .90, emerged as significant predictors of being classified in a higher suicide-risk category. (Table 4).
DISCUSSION AND CONCLUSION
The present study offers partial yet clinically meaningful evidence of the effectiveness of the DBT-MXAU skills program in Mexican secondary-school settings. Consistent with DBT theory (Linehan, 1993), global suicide-risk scores declined with medium effect sizes (Z = −2.84, p = .005, r = .40), as did checklist-based risk (Z = −2.71, p = .007, r = .38). These reductions meetCohen’s (1988) threshold for clinically relevant change.
Improvements in emotion regulation skills emerged in parallel with risk reduction. Global emotional intelligence, clarity, and repair each increased with medium effect sizes (Zs = −2.42 to −2.75, rs = .30 –.36), while post-intervention correlations showed that greater emotional clarity and repair were modestly yet significantly associated with lower suicide risk (for example, clarity with crisis risk: ρ = −.35, p = .009). These findings support the biosocial model’s contention that the ability to label and modulate emotional states buffers suicidal impulses. Contrary to expectations, self-reported frequency of DBT-skills use neither increased significantly (Z = −.76, p = .445, r = .10) nor predicted lower risk (ρ = −.01, p = .964). The absence of a protective association suggests that raw frequency counts fail to capture the quality of skill implementation, as noted in a previous study distinguishing declarative knowledge from behavioral competence (Neacsiu et al., 2014).
Program effects appeared consistent across geographic contexts. Results revealed only trivial post-intervention differences between the four participating cities (η2;_H ≤ .08), implying that DBT-MXAU achieves a comparable impact on diverse urban settings and may therefore be scalable within the national school system. Multivariate results, however, were constrained by a pronounced floor effect: approximately 90% of adolescents were classified in the “no risk” category after treatment, leaving insufficient variance for the ordinal logistic models. Neither city of residence (OR = .92, 95, CI .33, 2.57) nor the combination of post-program skills frequency (OR = 1.04, CI .98, 1.09) and emotional repair (OR = .90, CI .80, 1.02) predicted higher risk categories, and two-thirds of the predictor–outcome cells were empty, further reducing statistical power. Future research using randomized controlled trials (RCTs) will be necessary to confirm these findings and evaluate the impact of the intervention more effectively.
Several limitations temper the interpretation of these findings. First, the floor effect restricted both the detection of predictors and the estimation of effect sizes, indicating a need for samples with greater baseline variability in suicide risk. Second, reliance on self-reporting may have introduced social-desirability bias and recall error, particularly in the frequency-of-skills measure. Third, the pre-post design without follow-up makes it impossible to draw conclusions about gains maintenance or the temporal ordering of mechanisms (skill use → improved regulation → reduced risk). Fourth, small site-level samples limited the ability to conduct more granular moderation analyses. Fifth, the study did not control for potentially influential social variables (such as socioeconomic status, family environment, or previous mental health support), which may have affected both baseline risk levels and the response to the intervention. Future studies should account for these factors to clarify the specific impact of the DBT-MXAU program.
Despite these constraints, the results have meaningful implications for practice and future research. Enhancing in-vivo coaching, performance feedback, and ecological assessments could help translate skill frequency into functional mastery and capture real-time deployment. Longitudinal designs testing mediational chains between changes in skill competence, emotion regulation, and suicide risk would clarify causal pathways. Larger, multi-site samples or cluster-randomized trials could alleviate power limitations and allow the examination of school-level moderators.