INTRODUCTION
Attention deficit hyperactivity disorder (ADHD) is a common disorder present across cultures, with symptoms indicative of ADHD going back to childhood. Researchers have described ADHD as a neuropsychiatric disorder comprising inattention, motor hyperactivity, maladaptive impulsivity, and emotional dysregulation. In addition, ADHD causes negative consequences in every aspect of life (Jacob et al., 2016) and has been widely studied in the general population. Studies have estimated a 2.5% prevalence of ADHD in the adult population (Deberdt et al., 2015; Jacobsson et al., 2021; Nylander et al., 2009; Simon et al., 2009). Although many studies have suggested that ADHD has its roots in biological factors as a neurodevelopmental condition, it can manifest in various features and may include personality traits, such as neuroticism and impulsivity (Costa & McCrae, 1995; Nigg et al., 2020). Patients with ADHD often have other psychiatric disorders, such as mood, anxiety, personality, and substance disorders (Kessler et al., 2006; Matthies & Philipsen, 2014; Reimherr et al., 2015). Additional conditions include pathological personality traits such as emotional dysregulation, distractibility, irresponsibility, risktaking, and impulsivity. However, there are limitations in the literature on ADHD-personality disorder connections in the Diagnostic and Statistical Manuel of Mental Disorders, Fifth Edition (DSM-5) and International Classification of Diseases and Related Health Problems-11 (ICD-11) models (Jacobsson et al., 2021).
Studies have shown that ADHD patients often have personality disorders in adulthood (Simon et al., 2009). Although there are often confusing or vague explanations regarding methodological processes for sample characteristics, some researchers have reported percentages of personality disorder diagnoses in adult ADHD patients ranging from 10 to 75%. Researchers have also found a higher percentage of cluster B and a lower percentage of cluster C personality disorders (Anckarsäter et al., 2006; Biederman et al., 1993; Fischer et al., 2002; Mannuzza et al., 1991; Matthies & Philipsen, 2016). Some studies on adult ADHD have evaluated patients diagnosed with personality disorders according to the DSM system. Researchers have found that patients with ADHD often have borderline and antisocial personality disorders. Although there is reason to believe that ADHD and personality disorders may share etiological mechanisms, it is not easy to explain the developmental pathways involved (Matthies & Philipsen, 2016).
Definitions of narcissism in the literature are often conflicting. The disorder is difficult to define because it comprises a broad set of symptoms. There are currently two axes of distinction. The first divides narcissism into two categories by symptom severity: the healthy type and the clinical (dysfunctional) type. Some researchers define the healthy type as a functional and sometimes advantageous personality trait (Emmons, 1984). Characteristics of this axis include high self-esteem, deficiencies in interpersonal relationships, a likelihood of career success, and low empathy. The clinical type is almost synonymous with Narcissistic Personality disorder (NPD). Characteristics of this axis include a fixed, inflexible pattern of self-importance and belief in one’s uniqueness, an excessive need for admiration, and a lack of empathy, as diagnosed according to the DSM system (Jankowiak-Siuda & Zajkowski, 2013). The second axis includes grandiose and vulnerable narcissism (Wink, 1991), also known as overt and covert narcissism (Jankowiak-Siuda & Zajkowski, 2013).
Anckarsäter et al. have also highlighted the relationship between narcissistic personality disorder and ADHD. They have examined individuals with ADHD particularly predisposed to Cluster B personality disorders, comprising antisocial, narcissistic, and histrionic personality disorder. They argue that these personality disorders and ADHD may share common developmental pathways and disturbed emotional processes (Anckarsäter et al., 2006; Helgeland et al., 2005). One study has suggested that ADHD is associated with Cluster B personality disorders. Surprisingly for ADHD researchers, who have acknowledged the connection between ADHD and personality disorders, some scholars have found that the most prevalent personality disorders are narcissistic personality disorder in males and histrionic personality disorder in females. They have included 910 patients with adult ADHD (452 females and 458 males) (Jacob et al., 2016). These findings have generated intriguing data in the psychiatric field, because they underline the strong association between ADHD and narcissistic personality disorder. Nevertheless, studies in this area are as yet extremely limited.
Certain areas in the definition of empathy must be addressed. In the emotional domain, empathy is understood as the ability to share, understand, and co-experience the emotions of others (Wink, 1991; Stotland, 1969). From a cognitive perspective, empathy is the ability to imagine and understand the feelings and motivations of others (Davis et al.,1996; Eisenberg & Strayer, 1987; Ickes et al., 2000). Some authors have expanded the definition, equating it with mentalizing. These authors have also described it as the ability to be consciously aware of the thoughts, intentions, and desires of others (Frith & Frith, 2003).
Individuals experience social cognition as a process of empathic capacity enhancing the quality of social interactions. Some authors have suggested that adults with ADHD experience difficulty in facial emotion/affect processing and recognition (Ibáñez et al., 2011; Marsh & Williams, 2006; Miller et al., 2011). Others, however, have not reported empathy and social cognition deficits in patients with adult ADHD (Bora & Pantelis, 2016; Gonzalez-Gadea et al., 2013). Studies on empathy in patients with adult ADHD are both contradictory and inconsistent. Nevertheless, the social cognition and empathy process has received a great deal of attention in various ADHD studies. In addition, some studies have reported that autism spectrum disorders and ADHD show overlap in social dysfunctions, highlighting the relationship between ADHD symptoms and the empathizing–systemizing cognitive style (Groen et al., 2018).
This study investigated a set of factors regarding narcissism and empathy in adult ADHD. Our aim in this study was to examine ADHD symptoms, narcissism, and empathy levels in ADHD patients and the control group. Our main argument is that patients with ADHD have a significantly higher level of narcissism and a lower level of empathy. We also suggest that there is a significant relationship between symptom severity and narcissism levels in individuals with ADHD.
METHOD
Participants
In this cross-sectional study, researchers drew the study samples from patients attending the psychiatry clinics of the Bağcılar Training and Research Hospital (Istanbul, Turkey) and the Prof. Dr. Ilhan Varank Sancaktepe Training and Research Hospital (Istanbul, Turkey). Patients were diagnosed with Attention Deficiency and Hyperactivity Disorder based on the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5) criteria, which was confirmed by two senior psychiatrists (American Psychiatric Association, 2013). Initially, 120 patients and forty-four healthy controls were identified. Researchers included patients who did not have a history of psychotropic drug usage or who had stopped using at least three months prior to the beginning of the study. The exclusion criteria for the patient group were co-existing psychiatric disorders; mental retardation; being under the age of 18 and having a history of any neurological disease that could prevent communication such as organic mental disorders, head trauma, dementia, or epilepsy. Clinicians excluded twenty-five patients from the study because they were diagnosed with another comorbid mental disorder according to DSM-5. After applying the inclusion-exclusion criteria, researchers included patients (fifty-two men and forty-two women) with ADHD. They also formed a comparison group consisting of forty-four healthy controls (sixteen men and twenty-eight women). This group consisted of subjects who did not have a psychiatric or neurological disorder, were aged over 18 years, and agreed to participate in the study. During the selection process, efforts were made to match the groups for age and gender to ensure comparability. Although exact numerical equality was not achieved, statistical analyses confirmed no significant differences between the groups in terms of age and gender, minimizing potential demographic variability in the study.
Informed consent was obtained from all patients included in the study. A semi-structured sociodemographic and clinical data form and Adult Attention Deficit Hyperactivity Disorder Self-Report Scale (ASRS), Pathological Narcissism Inventory (PNI), and Empathy Quotient (EQ-60) scores were administered to all participants on admission.
Measurements
The semi-structured sociodemographic and clinical data form records participant characteristics such as age, gender, and clinical data. The Pathological Narcissism Inventory (PNI) is a 6-point Likert-type self-report scale developed by Pincus et al. (2009) to assess vulnerable and grandiose narcissism. The fifty-two item scale evaluates narcissism through two upper factors and seven sub-factors, including three for vulnerable narcissism and four for grandiose narcissism. The validity and reliability of the Turkish version were confirmed by Sen and Barıskın (2019), with Cronbach’s alpha reliability at .93 and test-retest reliability coefficient at r = .91. The Adult ADHD Self-Report Scale (ASRS), comprising eighteen items scored from one to four, was designed by the World Health Organization to screen for ADHD symptoms in adults and validated by Doğan et al. (2009) in the Turkish version. The Empathy Quotient (EQ-60), developed by Lawrence et al. (2004), measures empathy through forty questions and twenty distractors. The reliability and validity of the Turkish version were assessed by Bora and Baysan (2009).
Statistical analysis
Study data were analyzed with the SPSS 25.0 for Mac OS (Armonk, NY: IBM Corp.). The Kolmogorov-Smirnov test was used to determine whether the distribution of numerical data was normal before further analysis. Accordingly, chi-square, ANOVA and Student’s t-test were utilized to compare categorical and continuous variables between groups. The relationships among data were determined with the Pearson Correlation test. Linear regression analysis was undertaken to determine the independent variables predicting effects on narcissistic characteristics in ADHD patients: a p-value < .05 was considered significant.
Ethical considerations
Ethics committee approval was obtained for this research at the Bağcılar Health Sciences University Training and Research Hospital Ethics Committee on June 12, 2020, with decision number 2020.06.1.07.078.
RESULTS
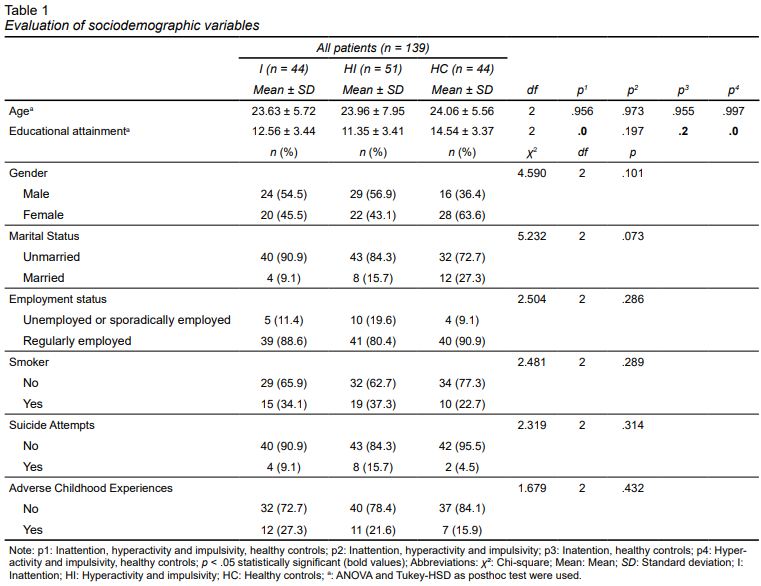
A comparison of the sociodemographic data of patients between groups is shown in Table 1. According to the sub-diagnosis of ADHD, forty-four patients were in the inattention group (I), fifty-one were in the hyperactivity and impulsivity (HI) group, and forty-four were in the healthy control (HC) group. Among the study participants, the mean age of the inattention group was 23.63 ± 5.72, the mean age of the hyperactivity and impulsivity group was 23.96 ± 7.95, and the mean age of the healthy control group was 24.06 ± 5.56, with no statistically significant difference being found. (p > .05). Educational achievement was significantly lower in the inattention, hyperactivity, and impulsivity groups than in the healthy control group (p = 0). There was no statistically significant difference between groups in terms of gender (χ2 = 4.590, p = .101). The normality of the data was assessed using the Kolmogorov-Smirnov test. The results showed that total ADHD (p = .210), narcissism (p = .230), and empathy scores (p = .059) did not deviate significantly from normality.
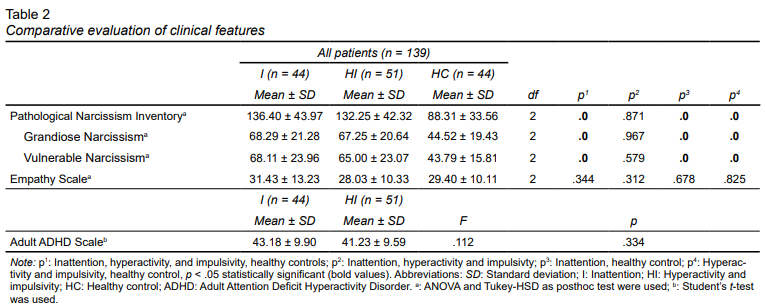
The evaluation of clinical features is shown in Table 2. There is a statistically significant difference between the three groups in the PNI scores (p = .001). PNI scores were significantly higher in both the inattention group (p = .001) and the hyperactivity and impulsivity group (p = .001) than in the healthy control group. In the pathological narcissism inventory, narcissistic grandiosity and narcissistic vulnerability subgroup scores were found to be significantly higher in the inattention, and hyperactivity and impulsivity groups than in the healthy control group (p = 0).
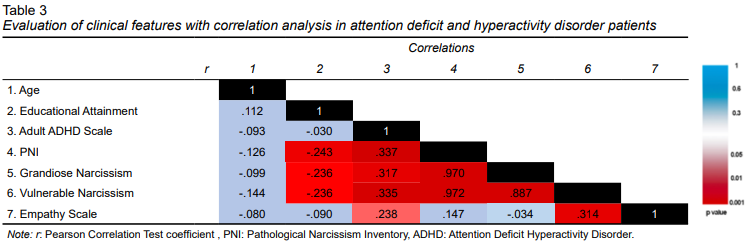
The relationship between the sociodemographic and clinical characteristics of participants is shown in the correlation chart in Table 3. There is a negative correlation between educational attainment and PNI score (r = -.243, p < .01), narcissistic grandiosity score (r = -.236, p < .01), and Narcissistic vulnerability score (r = -.236, p < .01). The Adult ADHD Scale score was positively correlated with the PNI score (r = .337, p < .01), Narcissistic grandiosity score (r = .317, p < .01), Narcissistic vulnerability score (r = .335, p < .01), and Empathy Scale score (r = .238, p < .05). There is a positive correlation between the Narcissistic grandiosity score and the Narcissistic vulnerability score (r = .887, p < .01) and between the narcissistic vulnerability score and the Empathy Scale score (r = .314, p < .01).
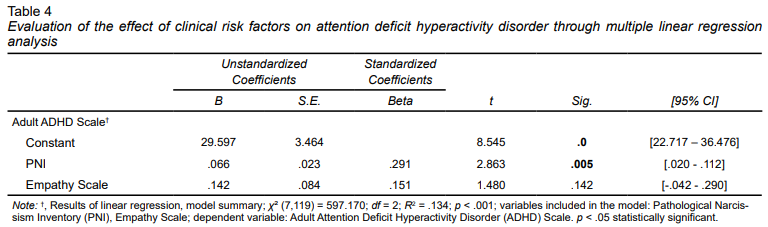
In Table 4, the effect of clinical risk factors on attention deficit hyperactivity disorder was evaluated by multiple linear regression analysis. The PNI scale and the Empathy scale were determined as the parameters to be evaluated in relation to ADHD in the model. A significant regression model was obtained (R2 = .134; χ2 (7.119) = 597.170; p < .001) and narcissistic features (β = .31, p < .05) were significantly associated with ADHD severity.
DISCUSSION AND CONCLUSION
This study provides a review of the research suggesting that pathological narcissism, adult ADHD, and empathy may be linked. The researchers analyzed the role of narcissism and empathy levels in mediating ADHD severity in the context of an overlapping phenomenological system. To summarize results, researchers found that patients with ADHD had higher narcissism scores than the healthy control group. However, they did not find a significant difference between the inattention group and the hyperactivity and impulsivity groups in terms of PNI scores. Unexpectedly, we did not find statistically significant differences in Empathy Scale scores between the inattention, hyperactivity-impulsivity, and healthy control groups. We also found that narcissistic features were significantly associated with ADHD severity in the logistic regression analysis model.
The severity symptoms of adult ADHD that may be associated with narcissism levels in this disorder were not evaluated in this article. It is tempting, though, to speculate as to the importance of personality traits and personality disorders. Patients with adult ADHD can have a combination of personality traits and personality disorders. For example, Bernardi et al. have reported that patients with ADHD often have borderline personality disorder and narcissistic personality disorder (Bernardi et al., 2012). Fossati et al. have also reported an association between childhood manifestation of ADHD and adult borderline personality disorder diagnosis (Fossati et al., 2002). In addition, Jacob et al. have found that the most prevalent personality disorders are narcissistic personality disorder in males and histrionic personality disorder in females (Jacob et al., 2016). In this study, we found extremely high narcissistic scores in patients with adult ADHD. It is suggested that the specific phenomenology of adult ADHD be more carefully evaluated for narcissistic pathology in these clinical findings.Moreover, we hypothesize that patients with adult ADHD with high levels of narcissism may have severe clinical disorders. Further evaluation of narcissistic pathology and personality disorder is required. We suggest that the increased narcissistic pathology seen in adult ADHD patients, particularly the grandiose or vulnerable narcissistic subtypes, are likely to be key mechanisms underlying the clinical disturbances demonstrated in narcissistic pathology.
We suggest that ADHD may occur before the narcissistic personality develops. We also posit that this developmental process is not easy to understand. The two disorders may begin in early childhood. But earlier onset of ADHD symptoms would appear to be more logical. Further investigation of candidates for these shared risk factors has focused predominantly on certain levels. Jacob et al. have demonstrated the relevance of Gene × Environment interactions in the pathogenesis of personality disorders and adult ADHD (Jacob et al., 2010). Jakob et al. have also suggested that personality transformations may be a result of adult ADHD and that the symptoms cause enduring psychological stress. The observed symptoms of personality disorders in adult ADHD patients may reflect a specific type of coping strategies (Jacob et al., 2007, 2016).
In the emotional realm, authors often describe empathy as the ability to share and experience the emotions of others (Davis et al., 1996; Eisenberg & Strayer, 1987; Stotland, 1969). From a cognitive perspective, empathy is the capacity to imagine and understand the feelings and motives of other people (Batson, 2009; Decety & Jackson, 2004; Decety & Svetlova, 2012; Ickes et al., 2000) . It also includes the ability to be consciously aware of their thoughts, intentions, and desires, known as mentalization (Frith & Frith, 2003) or possessing theory of mind (Decety & Jackson, 2004; Premack & Woodruff, 1978). When we evaluate the literature, we notice that empathy has a multifaceted conceptual framework. The literature brings together all the perspectives mentioned, describing empathy as a complex process (Davis et al., 1996; Ickes et al., 2000). Groen et al. studied cognitive and emotional empathy in adult ADHD, finding low emotional empathy scores. They demonstrated that ADHD traits were related to the emotional aspect of empathy. But they did not find the more complex aspects of empathy in patients with adult ADHD (Groen et al., 2018). Some authors have pointed out the problems adults with ADHD experience with facial emotion/affect processing and recognition (Miller et al., 2011). Other authors, however, have not reported empathy or social cognition deficits in patients with adult ADHD (Bora & Pantelis, 2016; Gonzalez-Gadea et al., 2013). Moreover, some studies report an overlap between autism spectrum disorders and ADHD in social dysfunction, and a link between ADHD symptoms and the empathizing–systemizing cognitive style (Groen et al., 2018). We did not find statistically significant empathy scores in the inattention, hyperactivity-impulsivity, and healthy control groups. When we evaluated them retrospectively, we observed contradictions. Many authors state that narcissistic pathology results from a lack of empathy. There are two types of narcissism: grandiose and vulnerable (Wink, 1991), alternatively known as overt and covert (Jankowiak-Siuda & Zajkowski, 2013). High levels of extraversion, self-confidence, self-esteem, exhibitionism, and aggression characterize the grandiose type. Conversely, introversion, low self-esteem, anxiety, and high susceptibility to traumas are associated with the vulnerable type (Jankowiak-Siuda & Zajkowski, 2013; Pincus et al., 2009; Rose, 2002.; Wink, 1991). Many studies have shown that the traits associated with all narcissism subtypes are selfishness, disregarding others, self-centeredness, and low empathy (Jankowiak-Siuda & Zajkowski, 2013). The observation that adult ADHD and empathic capacity could be associated with altered narcissistic pathology suggests that emotional and cognitive empathy may influence the severity of ADHD in which the pathologic system plays a role. The relationship between adult ADHD, narcissism, and empathy requires further research.
This study has certain limitations that should be considered when interpreting results. Although efforts were made to match groups for age and gender, exact numerical equivalence could not be ensured. Statistical analyses indicated no significant differences between the groups in these variables, yet potential demographic influences cannot be ruled out. Additionally, the unequal sample sizes across groups may have affected the statistical power of certain analyses. Finally, slight differences in gender distribution may have influenced outcomes related to gender-specific characteristics, warranting cautious interpretation of results.
This study suggests that the increased level of narcissistic pathology seen in patients with adult ADHD, particularly in the inattention and hyperactivity-impulsivity subtypes, is probably related to the severity of ADHD. Whether the high level of narcissistic pathology associated with adult ADHD is specific to this disorder or symptoms of other disorders requires further clarification. The relationship between adult ADHD and narcissism also warrants further research. Equally important is a better understanding of treatments based on psychopharmacology and psychotherapy. This research underlinesthe significance of therapies concentrating onnarcissistic pathology.