INTRODUCTION
In 2020, the world faced a serious public health crisis triggered by a novel coronavirus, SARS-CoV-2. The virus reached catastrophic proportions, spreading rapidly across six continents and causing majorsocial, economic, political, and health impacts (Jakovljevic, 2020). The pandemic exacerbated symptoms and psychological disorders such as loneliness (Van Tilburg et al., 2021), posttraumatic stress disorder (PTSD) (González-Sanguino et al., 2021), depression, and anxiety (González-Sanguino et al., 2021; Rettie & Daniels, 2021). The latter was even higher in at-risk groups for COVID-19, such as older adults (Rettie & Daniels, 2021).
The World Health Organization [WHO] (2021) recognized an infodemic as a potentially lethal response to the pandemic due to its catastrophic effects worldwide (Zarocostas, 2020). The term “infodemic” can be defined as an overload of information, regardless of whether it is true, related to a specific subject, making it difficult to obtain reliable sources and guidance, which increases exponentially in a short time (WHO, 2021).
In the age of digital information, infodemics are intensified by social networks, reaching a large number of people (Bridgman et al., 2020). Although patterns of information sharing on the internet have been studied for years, it was only with the COVID-19 pandemic that the first infodemic was recognized (Zarocostas, 2020). There is therefore still a dearth of evidence on the effects of this phenomenon on the population (Ahmad & Murad, 2020; Bridgman et al., 2020; Delgado et al., 2021). Nevertheless, it is known that sharing incorrect information encourages misinformation, triggering serious consequences such as death, xenophobia, discrimination, ideological polarization, and racism.
In Brazil, the political context compounded the pandemic scenario, leading to the emergence of conspiracy theories and misinterpretations of data. This scenario deteriorated as anti-science permeated the discourse and actions of certain government representatives. At this point, the repercussions of the infodemic on the mental health of older adults were evident. Studies conducted on the adult population revealed an increase in cases of depression associated with excessive information, as well as a recurrence of cases of depression caused by negative information on Covid-19 (Delgado et al., 2021; Kitamura et al., 2022).
The need to understand the effects of the infodemic on society goes beyond the current moment, as other infodemics are likely to emerge, linked to new epidemics, tragedies, terrorism, and climate catastrophes (Jakovljevic, 2020). It is therefore necessary to examine the phenomenon in detail.
Due to the lack of instruments for tracking or measuring symptoms and psychological disorders associated with infodemics, little is known about their effects on mental health. To explore this relationship, some studies have used instruments designed to assess psychological problems. These include those related to mental distress (4-item Patient Health Questionnaire, PHQ-4) and psychiatric disorders (Generalized Anxiety Disorder Scale—GAD-7), to associate the results with the infodemic. However, the use of instruments developed for the evaluation of other phenomena is suboptimal for the detection of infodemic disorder, leading to significant measurement problems. The infodemic should be evaluated using instruments specifically designed and validated for this purpose.
There is currently a lack of specific instruments to measure the effects of infodemics on the mental health of older adults. The objective of the present study was therefore to construct and analyze the internal structure validity and reliability of the Infodemic Signs and Symptoms Scale (ISSS) in older adults.
METHOD
This was a psychometric study of the construction and validation of a measurement instrument. The protocol was approved by the Human Research Ethics Committee (CEP Opinion No. 4,134,050) for national and international regulations for human research in a virtual setting. It is part of an international multicenter study currently under development, the “COVID-19 infodemic and its effects on the mental health of older adults during and after the pandemic: A multicenter study in Brazil/Chile/Peru/Colombia/Mexico and Portugal.” It seeks to analyze the relationship between the COVID-19 infodemic and the mental health of older adults.
To conduct the study, the ISSS instrument was administered to 3,003 older adults (aged 60 years old) from various regions of Brazil who provided their informed consent. The sample size calculation was determined on the basis of the psychometric principles of sample composition, considering at least ten respondents per item in the instrument (Hair, 1998). To participate in the study, subjects had to be able to read and fill in the forms online or answer interviewers by telephone. Older adults who resided in a long-term care facility were excluded because institutionalization can contribute to the development or worsening of mental distress. Subjects who declared that they were unable to answer the questionnaire using digital media or even by phone were excluded, Questionnaires with blank fields were omitted from the analysis.
Data collection took place remotely between July 2020 and March 2021. Instruments were administered online (web survey) or by phone to include older adults with limited knowledge of or access to technology.
Potential participants were invited by a web survey link sent through social media (Whatsapp, Facebook and Instagram) and/or email and/or telephone, using the virtual snowball strategy (Costa, 2018). To increase the representativeness of the sample, in addition the virtual snowball strategy, the link was shared with scientific societies of geriatrics and gerontology and retiree associations. In addition, phone calls were made to older adults, during which they were asked if they used social media. If so, they could choose whether to answer the questionnaire by telephone or to receive the link through social networks and/or e-mail.
Once they had accessed the link, older adults were asked to choose whether or not to accept the digital informed consent form (ICF). If a person preferred to participate in the study by telephone, they received an informed consent form from the researcher by email or social media. Only those who agreed to participate in the study had access to the web survey questions. At the end of the questionnaire, respondents were asked to forward or share a link with their network of contacts. After they had given their informed consent, they answered sociodemographic questions and questions related to the ISSS.
The ISSS was developed to track signs and symptoms of psychological distress associated with exposure to information about socially critical events (such as epidemics, terrorism and climate crisis). The ISSS was developed on the basis of the scientific literature on the main psychological problems and disorders caused or aggravated by pandemics and epidemics. These include stress (Czeisler et al., 2021; Shanahan et al., 2022), fear (Broche-Pérez et al., 2022; Dsouza et al., 2020; Fitzpatrick et al., 2020), and anxiety (Czeisler et al., 2021; Hou et al., 2020; Tang et al., 2021). Other aspects include substance abuse (Czeisler et al., 2021; Sun et al., 2020), depression (Czeisler et al., 2021; Hou et al., 2020; Tang et al., 2021) and suicidal ideation (Czeisler et al., 2021; Dsouza et al., 2020).
On the basis of the literature review, a 34-item scale was designed for older adults aged 60 years or over. Items are presented at random, and respondents are asked to indicate, either on their own or with the help of the interviewer, how often in the past fourteen days they experienced each of the signs or symptoms mentioned as a result of exposure to information about COVID-19. Items are measured on a four-point Likert-type scale (0—Never; 1—Rarely; 2—Sometimes; and 3— Often). The total score, calculated as the sum of the items, ranges from zero to 102. Higher scores indicate a greater burden of psychological distress. The cutoff point used was 67/68, considering the 95th percentile of the raw score.
The statement provided in the scale was: “In the past fourteen days, information on COVID-19 has affected me,” and the thirty-four items given below. These include Lack of hope or pessimism; Cold sweat or chills; Irritation; Reluctance to carry out my daily activities; Fear of getting sick; Nervousness; Panic; Increased alcohol or tobacco use and Decreased desire for sex. Other items were Fear of dying; Digestive problems; Dry mouth; Lack of interest in daily activities; Lack of energy; Chest tightness; Concern; Use of illegal substances; Wish to die; Anxiety; Difficulty breathing; and Sadness. Still others include Non-specific fear; Discouragement; Anger; Trembling; Headache; Muscle aches; Sleep problems; Nutritional problems; Palpitation; Tiredness; Fear that loved ones (family, friends, etc.) will die; Use of psychotropic drugs (such as sleeping pills and/or anxiety) and Desire to be alone. The variables comprising the various dimensions are drawn from studies published during the pandemic. They measured and analyzed the impact of the infodemic on the mental health of the population, as well as a review study implemented and published by the research group.
The dependent variable was the total and per item ISSS score. For the characterization of the sample, age, gender, marital status, education, race/color, cohabitation and residential area, health services used, income and change in income during the pandemic were considered independent variables. To analyze the relationship between ISSS and other variables, the 15-item version of the Geriatric Depression Scale, (GDS-15) (Almeida & Almeida, 1999) and the Geriatric Anxiety Inventory (GAI) (Martiny et al., 2011; Massena, 2014) were administered.
The treatment procedures and descriptive data analyses were undertaken based on the sociodemographic characterization of the participants. Descriptive analyses were performed to characterize the sample, and results were reported as frequencies and measures of central tendency and distribution. Characterization analyses were performed using SPSS Statistics 23.
Following the validation steps, items were designed based on theoretical studies conducted by researchers at the multicenter study, which provided the opportunity to extract questions to create the scale. The Delphi method was used to validate the content, and the item bank was evaluated by experts from the multicenter project. Another phase comprised the pre-test, in which the older adult’s understanding of the scale items was assessed. Approximately 80% of the older adults were drawn from research centers.
Evidence of the internal structure validity was obtained through exploratory factor analysis (EFA) and confirmatory factor analysis (CFA) using the Factor 12.03.01 software. EFA was performed using a polychoric correlation matrix (Gaskin & Happell, 2014). Measures of sample adequacy (Kaiser‒Meyer‒Olkin [KMO ≥ .70] and Bartlett index values [p < .05]) were calculated to test the factorability of the itemset. Parallel analysis was used to test dimensionality using the optimal implementation of parallel analysis based on minimum rank factor analysis (Timmerman & Lorenzo-Seva, 2011) and permutation with 500 random correlations (Buja & Eyuboglu, 1992). Data extraction was performed using the robust unweighted least squares (RULS) method (Costello & Osborne, 2005) with promin rotation (Lorenzo-Seva & Ferrando, 2019) if unidimensionality was not confirmed. The robustness of the test was determined from the association of a bootstrap with a sample extrapolation to 2,000 cases.
The goodness of fit of the model was analyzed based on the factor loadings (> .50) and communalities (> .40). The total explained variance (TEV) was set at 60% (Hair et al., 1998). In addition, unidimensionality evaluation indicators were adopted, namely, unidimensional congruence (UniCo) > .95, explained common variation (ECV) > .80 and mean of item residual absolute loadings (MIREAL) < .30 (Ferrando & Lorenzo-Seva, 2017).
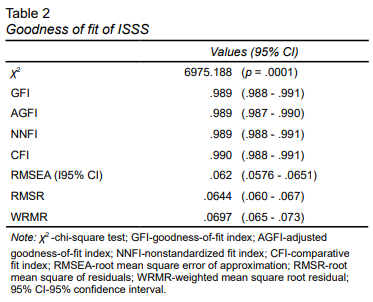
The parameters and respective reference values adopted to determine the fit of the model in the CFA were the NNFI (non-normed fit index > .95), CFI (comparative fit index > .95), GFI (goodness-of-fit index > .95), AGFI (adjusted goodness-of-git index > .95), RMSEA (root mean square error of approximation < .08), RMSR (root mean square of residuals < .08) and WRMR (weighted root mean square residual < 1.0) (Sivo et al., 2006).
Cronbach’s alpha and McDonald’s omega indicators were used to determine the reliability of the scale, with values greater than .70 for both indicating reliability. The replicability of the construct was assessed using the GH Index (Generalized GH Index > .80) (Hair et al., 1998). The quality and effectiveness of the factor estimation was established using the factor determination index (FDI > .904), the EAP marginal reliability (>.80), the sensitivity rate (SR > 2) and the expected percentage of actual differences (> 90%) (Lorenzo-Seva & Van Ginkel, 2016). The 95% confidence intervals for the analyzed indicators are presented.
RESULTS
A total of 3,003 participants completed the survey, answering the thirty-four items in the scale. In most cases (n = 2293; 76.3%), the instruments were administered online (web survey). In 23.7% of cases, they were administered by phone (n = 711).
From the sample of 3,003 participants, psychometric analyses were performed based on eighty-eight observations per item of the instrument. All response options were ticked (min = 0, max = 3). The skewness (83402.1) and kurtosis (394.5) for all items met the distribution requirements to perform EFA and CFA, as did the sample adequacy indices, which showed good levels of factorability (KMO = .97; Bartlett’s sphericity test df = 561 = 34421.7; p < .0001).
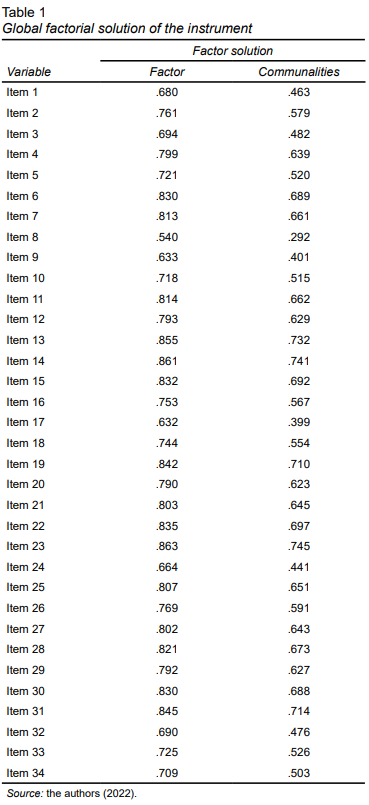
The parallel analysis indicated only one dimension in the instrument based on the 95th percentile, with a total explained variance of 60.8% of the latent variable. Unidimensionality was confirmed from the values obtained for the indicators UniCo (.984), ECV (.924) and MIREAL (.166). Factor loadings remained between .54 and .86 and the communalities remained above .40 for thirty-three of the thirty-four items. Although the communality of Item 8 was lower than the established cutoff, the item was not excluded due to its adequate factor loading and theoretical importance. Table 1 presents the global factor solution of the instrument.
The CFA results indicated a good fit of the model and an acceptable residual level.
The instrument has good reliability (Cronbach’s alpha = .97 and McDonald’s omega = .97) and excellent replicability of the construct, as evidenced by the GH index (latent = .982 and observed = .884). Evidence of the quality and efficacy of the measures showed high values for the FDI (.991) and EAP marginal reliability (.982), sensitivity rate (7.452), and the expected percentage of actual differences (98%).
DISCUSSION AND CONCLUSION
The impact of crises, pandemics and disasters is marked by sudden, unexpected change, usually involving the loss of material, social, and emotional resources. This exacerbates the signs and symptoms of mental distress, leading to an inability to cope with emergency situations. In these situations, people tend to overestimate risks, become anxious and afraid and have difficulty dealing with and adapting to environmental stressors (Zwielewski et al., 2020).
Short-term exposure to epidemic or pandemic situations can cause somatic complaints arising from states of emotional lability, social relationship issues and isolation, sleep pattern problems, and other behavioral manifestations. In the long term, these stressors can lead to posttraumatic stress disorder, anxiety, depression, excessive alcohol use, panic disorder and other conditions detrimental to social functioning and mental health (de Cassia, 2020).
Regarding the infodemic phenomenon, during the COVID-19 pandemic, the elderly population became vulnerable to being the targets of disinformation. This vulnerability is linked to the quantitative increase in information because the older population does not always follow recommendations regarding checking information amid the profusion of inaccurate news. This can either be due to a lack of digital or health literacy, key to controlling belief in misinformation, anxiety, and emotional instability triggered by the information or to cognitive processes linked to these behaviors. Unaware that this is misinformation, older adults may also unwittingly serve as disseminators of fake news in the information environment (Yabrude et al., 2020; Kitamura et al., 2022).
In addition to the risk of exposure to misinformation, this media-fueled distress impacts mental health, as misinformation can exacerbate stress responses, fear, and depression and anxiety disorders (Yabrude et al., 2020). It is therefore necessary to mitigate the way infodemics affect the mental health of the older population. Hou et al. (2020)evaluated the levels of anxiety and depression in 4,827 Chinese people aged 18 years or older (M = 32.3; SD = 10.0; 18-85 years). They associated the results with the frequency of exposure to news and information about COVID-19 on social networks in the previous week. Eighty-two percent of participants had been frequently exposed to information on social networks, which was associated with a high risk of clinically significant anxiety and combined depression and anxiety.
Riehm et al. (2020) conducted a study of over 6,000 US adults (M = 48.8; SD = .8 years). The results showed that the increase in time spent on social media and consulting traditional media sources (such as television, radio, and newspaper) to learn about COVID-19 were independently associated with increased mental stress.
Similarly, Sigurvinsdottir et al. (2020) found that the search for information on the pandemic on the internet was associated with more stress in participants. Importantly, the methodology used in the study did not make it possible to determine whether the search for information causes psychological symptoms or whether individuals experiencing negative feelings seek information, creating a type of feedback loop (Sigurvinsdottir et al., 202).
A study by Jungmann and Witthöft (2020) of German subjects (N = 1,615; M = 33.36 years; SD = 13.18) found a negative correlation between being informed about the pandemic and anxiety about the virus. For the authors, adaptive emotion regulation was a key moderator of this relationship. In contrast, pandemic cyberchondria (repeated and/or excessive internet searches related to the COVID-19 pandemic) was positively correlated with anxiety.
A study by Elhai et al. (2020) of 908 Chinese subjects (M = 40.37 years; SD = 9.27; 17-64 years) was conducted using standard instruments such as the Depression Anxiety Stress Scale-21 (DASS-21) and the Smartphone Addiction Scale – Short Version (SAS-SV) adapted to the context of the pandemic. The Generalized Anxiety Disorder Scale-7 (GAD-7), for example, was adapted by the authors for COVID-19 anxiety by providing the following context: “Over the last two weeks, how often have you been bothered by the following problems because of the coronavirus outbreak?” In addition, items assessing exposure to COVID-19 news were used. Among other results, Elhai et al. (2020)found that 11.67% had moderate depression, and 3.74% severe depression. 24.12% had moderate anxiety, and 6.83% severe anxiety; 7.93% had moderate COVID-19 anxiety and 2.64% severe COVID-19 anxiety; while 51.98% had problematic smartphone use. COVID-19 anxiety was positively correlated with depression and problematic smartphone use.
In this context, Kwiecinski (2019) analyzed the impact of information technologies. They assessed the levels of infoxication and nomophobia of higher education students through an analysis of concepts and foundations about infoxication and nomophobia, creating a psychometric scale to measure their levels in students. For this purpose, a mixed method study was conducted on the methodological development of the construction and validation of the psychometric instrument Psychometric Scale to Identify Levels of Infoxication and Nomophobia (Portuguese acronym EPININ).
The present study fills a gap, as there were no validated instruments for measuring the effects of infodemics on the mental health of older adults. The analyzed evidence indicates that the ISSS has good internal structure validity and reliability for measuring the signs and symptoms of infodemics in older adults. The set of thirty-four items, belonging to a single dimension, explains 60.8% of the phenomenon. The factor solution found shows good structure and a good fit. The analyses were performed using a contemporary theoretical model with robust techniques. It will be necessary to study the instrument further to refine the contents of the items with regard to the way they were constructed.
The instrument will assist in screening for mental distress in older adults caused by infodemics in emergency crisis contexts.
A brief version could be designed to optimize the applicability of the scale, The inclusion of lengthy instruments in comprehensive geriatric assessments (CGAs) could limit their use in practice and create biases due to items left blank by the participants.
One limitation of the study is the use of a web-based survey, leaving out a significant portion of people without access to the internet or social media, creating selection bias. The profile of the subjects displays certain characteristics mentioned above. These are not typical of the Brazilian population and could be interpreted as socioeconomic variables that protect against mental illness.